Généralité
L'hyperparathyroïdie est une affection clinique liée à la synthèse et à la sécrétion excessives de l'hormone parathyroïdienne.
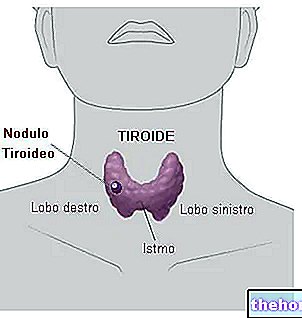
Il s'agit donc des glandes parathyroïdes, quatre petites glandes situées deux à deux sur la face dorsale de la thyroïde, semblables aux lentilles et responsables de la synthèse de l'hormone parathyroïdienne (PTH) et de sa libération dans le sang ; à son tour, cette hormone protéique exerce un effet hypercalcémique, augmentant la mobilisation du calcium des os, stimulant l'absorption intestinale (médiée par la vitamine D) et diminuant l'excrétion urinaire.
Pour cette raison, la plupart des formes d'hyperparathyroïdie s'accompagnent d'une augmentation de la concentration de calcium dans le sang, une condition connue sous le nom d'hypercalcémie.
Le rôle biologique de la paratharmone est contrecarré par la calcitonine qui, après avoir été synthétisée et sécrétée par la glande thyroïde, favorise le dépôt de calcium dans les os.
Connaissances

Causes
L'hyperparathyroïdie peut résulter de :
- sécrétion autonome et exagérée de parathyroïde par une ou plusieurs glandes parathyroïdes (hyperparathyroïdie primaire);
- sécrétion excessive d'hormone parathyroïdienne - en l'absence d'une maladie inhérente des glandes parathyroïdes - causée par la réponse à l'hypocalcémie (hyperparathyroïdie secondaire).
Hyperparathyroïdie primaire
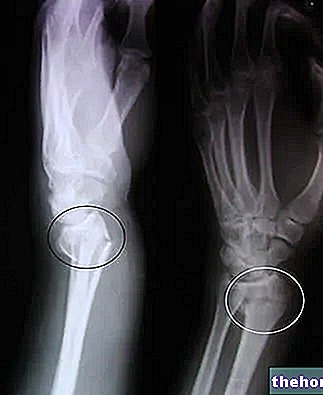
Dans 85 % des cas l'origine de l'hyperparathyroïdie primitive est liée à une tumeur bénigne (adénome) des glandes parathyroïdes.D'autres fois (14 % des cas) l'affection est liée à l'augmentation de volume d'une ou plusieurs glandes ; dans ces circonstances, on parle d'hyperplasie parathyroïdienne. Très rarement (1% des cas), à l'origine du problème se trouve plutôt une tumeur maligne, appelée carcinome parathyroïdien.Quelle que soit son origine, la sécrétion excessive d'hormone parathyroïdienne provoque une élévation du calcium dans le sang ; à long terme, les os ont tendance à se déminéraliser et à se fracturer facilement, tandis que la quantité de calcium alimentaire absorbée au niveau entérique a tendance à augmenter. Par conséquent, l'excrétion urinaire de calcium (bien que dans des conditions physiologiques l'hormone parathyroïdienne ait l'effet inverse) et de phosphore augmente également, exposant le sujet à un plus grand risque de calculs rénaux.
Hyperparathyroïdie secondaire
L'hyperparathyroïdie secondaire traduit l'hypersécrétion d'hormone parathyroïdienne en réponse à la diminution des taux de calcium dans l'organisme ; cette hyperactivité parathyroïdienne compensatrice - qui se traduit par une hyperplasie des mêmes glandes avec hypersécrétion d'hormone parathyroïdienne - peut donc être due à un apport alimentaire déficient en calcium et / ou de la vitamine D, ainsi qu'un défaut important de l'absorption intestinale du minéral (syndrome de malabsorption, comme cela se produit chez les coeliaques ou chez les individus souffrant de maladies inflammatoires intestinales chroniques). La cause la plus fréquente d'hyperparathyroïdie secondaire, du moins dans les pays industrialisés, est cependant représentée par « l'insuffisance rénale chronique ; en effet, on se souvient que le rein joue un rôle fondamental dans l'activation de la vitamine D. De plus, dans l'insuffisance rénale chronique l'augmentation dans la phosphatémie favorise une réduction supplémentaire et progressive du calcium.
Facteurs de risque
Le risque d'hyperparathyroïdie est légèrement plus élevé chez les femmes que chez les hommes (3 : 2), surtout dans les premières années après la ménopause. Cependant, même les personnes qui ne consomment pas suffisamment de calcium et de vitamine D dans leur alimentation sont plus à risque de développer la maladie. Enfin, l'hyperparathyroïdie touche le plus souvent les personnes atteintes de néoplasie endocrinienne multiple (maladie héréditaire rare), celles qui ont subi une radiothérapie dans la région du cou et les personnes sous traitement au lithium (un médicament souvent utilisé dans le traitement du trouble bipolaire).
Maladies des glandes parathyroïdes
Des problèmes avec la lecture de la vidéo ? Rechargez la vidéo de youtube.
- Aller à la page vidéo
- Aller à Destination Bien-être
- Regardez la vidéo sur youtube
Autres articles sur "Hyperparathyroïdie"
- Hyperparathyroïdie: symptômes et diagnostic
- Hyperparathyroïdie : traitement
- Hyperparathyroïdie - Médicaments pour le traitement de l'hyperparathyroïdie