Les symptômes de l'ischémie dépendent de l'organe et du tissu impliqués; cela signifie, par exemple, qu'une « ischémie cardiaque se présente avec un tableau symptomatologique différent d'une » ischémie cérébrale.
La survie et la récupération fonctionnelle après un épisode d'ischémie dépendent essentiellement de la rapidité du traitement.
.
L'oxygène et les nutriments sont des éléments fondamentaux pour la survie des cellules composant l'organisme humain ; en effet, leur absence prolongée (due par exemple à un manque d'intervention thérapeutique) déclenche un processus irréversible qui conduit à la mort (ou à la nécrose) de la organes et/ou tissus concernés.
L'ischémie est une maladie vasculaire, qui affecte principalement les artères.
Ischémie : quels sont les organes les plus touchés ?
Toute partie du corps peut souffrir d'ischémie.
Cependant, il existe des organes plus à risque que d'autres et qui, une fois atteints, peuvent avoir des conséquences graves ; les corps en question sont :
- Le cœur, qui peut développer une maladie connue sous le nom de cardiopathie ischémique, d'ischémie myocardique ou d'ischémie cardiaque ;
- Le cerveau, qui peut être victime d'ischémie cérébrale ;
- L'intestin, qui peut développer une ischémie intestinale ;
- Les extrémités des membres supérieurs ou inférieurs, qui peuvent subir l'ischémie dite périphérique.
Compte tenu de la fréquence plus élevée des phénomènes ischémiques dans les zones anatomiques susmentionnées, dans les prochains chapitres, l'article aura tendance à se référer aux types d'ischémie susmentionnés.
et l'interruption conséquente de l'apport sanguin aux organes et tissus garantis par les artères susmentionnées.Dans la plupart des cas, les événements obstructifs d'une « ischémie sont la conséquence d'une » embolie, d'une thrombose et d'événements traumatiques.
Classiquement, l'embolie et la thrombose sont associées à une ischémie myocardique, cérébrale et intestinale ; les événements traumatiques, quant à eux, sont liés à l'apparition d'ischémie périphérique au niveau des doigts ou des orteils.
Thrombose et embolie : que sont-ils en bref ?
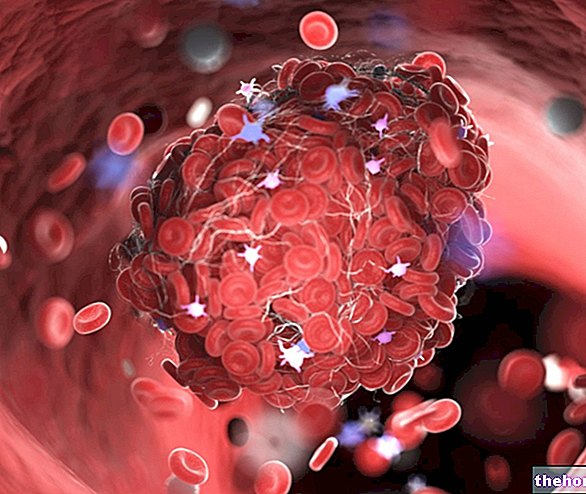
Le terme « thrombose » indique la présence d'un caillot sanguin, appelé thrombus, sur la paroi interne d'un vaisseau sanguin artériel ou veineux.
Le mot "embolie", en revanche, identifie la présence, dans le sang (donc dans les vaisseaux), d'un corps mobile d'origine sanguine ou non sanguine, qui prend le nom spécifique d'embole.
S'ils sont gros, les thrombus, ainsi que les emboles, peuvent obstruer les vaisseaux sanguins.
Ischémie : Facteurs de risque

De nombreuses conditions favorisent les phénomènes d'ischémie.
Parmi les nombreux facteurs de risque de cette maladie grave, ils méritent certainement une mention :
- Fibrillation auriculaire. Il s'agit d'une « arythmie, c'est-à-dire d'une » altération du rythme cardiaque.
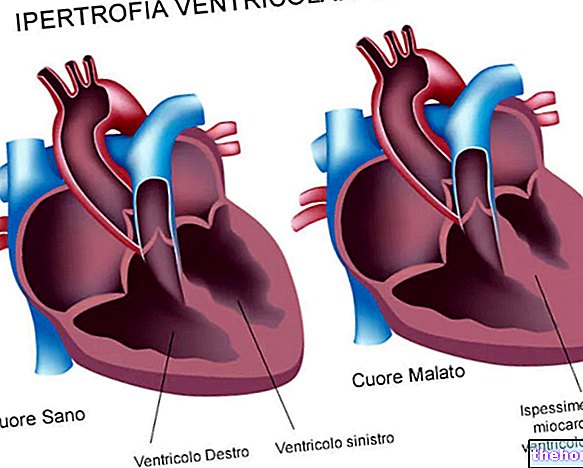
- Cardiomyopathies. Ce sont des pathologistes du muscle cardiaque (ou myocarde), en présence duquel le cœur fonctionne mal.
- Maladie coronarienne. Ce sont des maladies des artères coronaires, c'est-à-dire des vaisseaux artériels qui nourrissent et oxygènent le myocarde.
- Maladies de la valve mitrale. La valve mitrale est la valve cardiaque qui régule le passage du sang entre l'oreillette et le ventricule gauche.
- Diabète. C'est une maladie métabolique, qui en l'absence de traitement est à l'origine de nombreuses complications.
- Hypertension C'est l'augmentation chronique de la pression artérielle à des niveaux pathologiques.
- Hypotension due à un choc septique ou à une insuffisance cardiaque.
- Artériosclérose C'est le durcissement et l'épaississement de la paroi artérielle.
- Athérosclérose C'est une forme particulière d'athérosclérose, due à la présence d'athéromes (plaques de lipides, de protéines et de matière fibreuse).
- Hypercholestérolémie (cholestérol sanguin élevé) ou hypertriglycéridémie (triglycérides sanguins élevés).
- L'hypoglycémie est une réduction chronique de la glycémie à des niveaux pathologiques.
- L'âge avancé.
- Surpoids et obésité.
- Le mode de vie sédentaire.
- Fumée de cigarette.
- Thromboembolie veineuse. Indique la formation veineuse d'emboles qui, une fois arrivés au cœur, peuvent ensuite se propager au système artériel, créant des obstructions dangereuses.
- Maladie artérielle périphérique C'est l'obstruction des artères qui alimentent les membres, le tronc ou la tête.
- L'anémie falciforme.
- Le syndrome du défilé thoracique. C'est l'ensemble des symptômes et signes dérivant de la compression des vaisseaux sanguins et/ou des nerfs passant par le défilé thoracique.
- La compression des vaisseaux sanguins causée par la présence de tumeurs (effet de masse tumorale).
- L'exposition des membres à un froid excessif ou une mauvaise utilisation de la cryothérapie associée à l'application de bandages élastiques.
- La rupture sévère de nombreux vaisseaux sanguins.
- La rupture d'un anévrisme.
Ischémie aiguë et ischémie chronique
Une ischémie peut se présenter sous une forme aiguë ou chronique.
Ce qui distingue la forme aiguë de la forme chronique, c'est le fait que, dans la première, la réduction du débit sanguin est soudaine et soudaine, tandis que, dans la seconde, le même processus se produit progressivement.
Par la rapidité avec laquelle elle débute et avec laquelle elle donne lieu à des complications, l'ischémie aiguë représente une urgence médicale à traiter au plus vite.
Cela signifie qu'une « ischémie cardiaque présentera un tableau symptomatologique différent de celui d'une ischémie cérébrale ou d'une » ischémie périphérique.
Dans le corps humain, certains organes et tissus souffrent le plus d'une diminution de l'apport sanguin à leurs cellules.Le cœur, le cerveau et les reins, par exemple, sont des organes particulièrement sensibles au manque d'oxygène et de nutriments : déjà après 3-4 minutes, en fait, ils développent des dommages irréversibles (nécrose).
En revanche, il faut noter que tous les tissus et organes qui ont un métabolisme lent présentent les premières conséquences irréversibles après une période d'environ 20 minutes.
Malheureusement, certains cas d'ischémie sont asymptomatiques, ce qui signifie qu'ils ne présentent aucun symptôme. Ces situations peuvent être très dangereuses, car ceux qui en sont victimes ne réalisent pas ce qui leur arrive et ne se tournent pas rapidement vers les secours.
Ischémie cardiaque : qu'est-ce que c'est et les symptômes
Le terme « ischémie cardiaque » englobe deux pathologies très courantes, connues sous le nom d'angine de poitrine et d'infarctus du myocarde, dans lesquelles, suite à l'occlusion d'une ou plusieurs artères coronaires, un décalage entre la consommation et l'apport d'oxygène au myocarde se produit.
Dans l'angine de poitrine, le processus ischémique est temporaire/réversible et n'entraîne pas de dommages permanents (l'occlusion coronaire est temporaire).
Au contraire, dans l'infarctus du myocarde - également appelé crise cardiaque - l'ischémie est prolongée et entraîne une nécrose plus ou moins étendue du myocarde (dans ce cas, l'occlusion coronaire est durable dans le temps).
Clairement, du point de vue de la gravité, il existe une différence substantielle entre les deux affections : l'angine de poitrine est le signe d'une moindre souffrance cardiaque par rapport à l'infarctus du myocarde.
Les symptômes de l'angine de poitrine et de la crise cardiaque sont très similaires et se chevauchent presque ; ce qui change, c'est leur durée.
Les symptômes typiques de ces deux conditions comprennent :
- Douleur ou pression dans la poitrine
- Douleur qui, de la poitrine, peut irradier vers le dos, le bras, l'épaule, le cou, la mâchoire ou le ventre;
- Dyspnée, c'est-à-dire essoufflement ;
- Nausées avec ou sans vomissements;
- Limitations de la capacité physique. Par exemple, le patient se sent fatigué après un effort, même minime ;
- Palpitations ou rythmes cardiaques irréguliers (arythmies);
- Transpiration abondante.
Ischémie cérébrale : qu'est-ce que c'est et les symptômes

L'ischémie cérébrale est le processus pathologique qui caractérise deux affections certainement connues de la plupart : l'accident ischémique transitoire (ou AIT) et l'accident vasculaire cérébral ischémique.
Un AIT (également connu sous le nom de mini-AVC) est une « perturbation temporaire du flux sanguin vers le cerveau qui dure moins de 24 heures, sans conséquences permanentes.
Un AVC ischémique, en revanche, est une « interruption prolongée du flux sanguin cérébral, qui provoque des symptômes durant plus de 24 heures et une série de lésions cérébrales irréversibles.
Bien que l'AIT et l'AVC ischémique soient de gravité différente, ils présentent des symptômes très similaires, qui peuvent inclure :
- Paralysie et engourdissement du visage et des membres ;
- Difficulté à marcher, problèmes d'équilibre, déficits de coordination et tendance à tomber;
- Difficulté à parler et à comprendre
- Difficultés visuelles (vision double, vision floue, cécité soudaine, etc.);
- Taille anormale de la pupille et manque de réactivité de cette dernière aux variations de lumière ;
- Mal de tête;
- Vertiges;
- Confusion;
- Déficit de mémoire
- Nausées avec ou sans vomissements;
- La faiblesse;
- Altérations de l'état de conscience.
La succession de nombreux mini-AVC et de certains AVC ischémiques particuliers peut conduire à une forme de démence, connue sous le nom de démence vasculaire.
Ischémie intestinale : qu'est-ce que c'est et les symptômes
L'ischémie intestinale consiste en une diminution/interruption de l'apport sanguin à l'intestin, consécutive à une obstruction artérielle.
L'ischémie intestinale peut provoquer de violentes douleurs abdominales, des vomissements et/ou des diarrhées (souvent avec du sang).
Lorsque les dommages de l'ischémie intestinale sont permanents et qu'une nécrose de la section intestinale s'est produite, les médecins parlent plus correctement d'infarctus intestinal.
Pour plus d'informations : Ischémie intestinale : qu'est-ce que c'est, ses causes, ses symptômes et son traitementIschémie périphérique : qu'est-ce que c'est et les symptômes

« Ischémie périphérique » est le terme médical qui indique un apport sanguin insuffisant aux membres supérieurs ou inférieurs, en raison de l'obstruction d'un vaisseau artériel.
L'ischémie périphérique est généralement un phénomène aigu ; à ce titre, elle prend le deuxième nom d'ischémie aiguë des membres (ou ischémie aiguë des membres).
Les symptômes typiques de « l'ischémie aiguë des membres » sont : la douleur, la pâleur, la paresthésie, la paralysie et la perte de la thermorégulation normale (poïkilothermie).
Ischémie : quand contacter le médecin ?
Les formes les plus sévères d'ischémie nécessitent une intervention médicale immédiate, car la survie du patient est menacée.
Les médecins pensent que certains symptômes sont plus révélateurs d'une « ischémie sévère. Par exemple, ils considèrent un signe de danger extrême :
- Vomissements ou diarrhée sanglante;
- Douleur abdominale insupportable;
- Paralysie des membres ;
- Dyspnée au repos;
- Changements évidents dans les compétences visuelles ;
- Douleur intense dans la poitrine, ainsi qu'un fort sentiment de pression;
- L'incapacité de parler ou de comprendre ;
- Altérations de l'état de conscience.
Si ces contrôles s'avèrent insuffisants ou s'il est nécessaire d'approfondir la situation, il pourra également prescrire une échocardiographie, une radiographie pulmonaire et une « coronarographie ».
. C'est une procédure qui vous permet d'éliminer d'éventuels rétrécissements dans un vaisseau sanguin.La technique généralement utilisée pour ce type d'intervention est lo pose d'endoprothèse.
Le pontage artériel le plus connu est le pontage aorto-coronarien, mais il est important de rappeler aux lecteurs qu'il existe également des pontages artériels des membres inférieurs.
Il existe différentes techniques pour effectuer les opérations susmentionnées, certaines plus invasives que d'autres.
Ischémie : thérapies symptomatiques
Certains épisodes d'ischémie se prêtent également à certains traitements symptomatiques, c'est-à-dire ceux visant à améliorer le tableau symptomatologique.
Des exemples de traitements symptomatiques sont : les analgésiques (pour contrôler la douleur), les médicaments vasodilatateurs (pour augmenter le calibre des vaisseaux sanguins), les médicaments pour réduire la charge de travail du cœur (inhibiteurs calciques, IEC, nitrates et bêta-bloquants) et l'oxygène thérapie.
Ischémie : thérapies préventives
Les patients présentant une ischémie suite à une embolie ou une thrombose sont souvent des sujets prédisposés aux rechutes.
Pour réduire cette prédisposition, les médecins prescrivent aux patients un traitement anticoagulant au long cours, basé sur l'administration de médicaments tels que la warfarine ou l'héparine, et un traitement antiplaquettaire, qui implique l'utilisation d'agents antiplaquettaires tels que l'aspirine.
Ischémie et traitements invasifs : amputation
Les formes sévères d'ischémie périphérique nécessitent une intervention chirurgicale drastique avec des séquelles permanentes, telles que l'amputation du membre atteint.
Dans de telles situations, l'amputation est motivée par un processus de gangrène sèche ou humide, induit par le processus ischémique.
En médecine, le terme gangrène (ou gangrène) désigne un état pathologique caractérisé par la putréfaction massive d'un ou plusieurs tissus de l'organisme.
La gangrène nécessite une intervention médicale immédiate pour empêcher sa propagation aux tissus sains adjacents; cela explique la raison de l'« amputation : cette dernière, en fait, représente le seul moyen d'arrêter le processus de propagation de la gangrène elle-même ».
Ischémie cardiaque : les remèdes

En règle générale, le traitement de l'ischémie myocardique repose sur un ajustement (évidemment pour le mieux) du mode de vie et, selon que l'occlusion coronaire est légère ou sévère, sur un traitement médicamenteux ou chirurgical.
Médicaments pour le traitement de l'ischémie cardiaque
Parmi les médicaments utilisés dans le traitement de l'ischémie cardiaque, on note les suivants :
- Anticoagulants (par exemple héparine) et agents antiplaquettaires (par exemple aspirine).
- Nitroglycérine.
- Bêta-bloquants, inhibiteurs de l'ECA et antagonistes des récepteurs de l'angiotensine II.
- Statines.
Chirurgie de l'ischémie cardiaque
En ce qui concerne les actes chirurgicaux, il s'agit de :
- La greffe de pontage aorto-coronarien susmentionnée ;
- L"angioplastie avec pose d'endoprothèse coronaire.
Pour en savoir plus sur « le traitement de « l'ischémie cardiaque », nous vous recommandons de lire l'article dédié ici.
Ischémie cérébrale : les remèdes
Le traitement de l'ischémie cérébrale comprend certainement un traitement pharmacologique et, parfois, une thérapie chirurgicale ; de plus, une fois le flux sanguin rétabli, il offre également une voie de rééducation pour la récupération de toutes ces facultés motrices et cognitives compromises en raison de « l'événement vasculaire .
Médicaments pour le traitement de l'ischémie cérébrale
Les médicaments pour le traitement de l'ischémie cérébrale comprennent :
- Antithrombotiques (ou thrombolytiques) tels que l'aspirine ou l'activateur tissulaire du plasminogène recombinant (TPA).
- Les anticoagulants comme par exemple l'héparine, la warfarine, le clopidogrel ou le dipyridamole.
Chirurgie de l'ischémie cérébrale
Les principales interventions chirurgicales pouvant être adoptées en présence d'ischémie cérébrale sont :
- L'administration de la TPA directement in situ, par cathéter.
- Embolectomie ou thrombectomie.
- Endartériectomie carotidienne Il est à noter que cette option thérapeutique est utilisée lorsque l'empêchement à l'apport de sang vers le cerveau se situe au niveau des carotides.
- L"angioplastie avec pose d'endoprothèse.
Pour en savoir plus sur « le traitement de « l'ischémie cérébrale », nous vous recommandons de lire l'article dédié ici.
une alimentation régulière et saine et équilibrée, et qui exclut évidemment les mauvaises habitudes, comme le tabagisme ou l'abus d'alcool.