Edité par le Dr Andrea Gizdulich
introduction
La découverte de plus en plus fréquente de céphalées habituelles et persistantes chez les patients présentant des problèmes anatomiques et/ou fonctionnels affectant le système stomatognathique explique la nécessité d'inclure les céphalées de tension secondaires parmi les pathologies dentaires.Il ne faut pas non plus sous-estimer que la conscience d'un lien entre ces deux pathologies s'est également répandu parmi les médias de masse, influençant l'opinion publique. Comprendre les relations causales existant entre le système masticatoire et les céphalées secondaires nécessite une connaissance approfondie de la physiopathologie du système stomatognathique, partie initiale du système digestif mais aussi partie du système locomoteur.Doté d'un squelette osseux, d'articulations et d'un complexe et musculature variée possède une innervation et une proprioception riches largement dépendantes des deuxième et troisième branches du nerf trijumeau, ainsi que des organes spécifiques tels que les dents, situés dans les arcades maxillaire et mandibulaire.Certaines particularités confèrent à cet appareil des caractéristiques anatomiques et fonctionnelles uniques dans le corps humain : la mandibule, os unique et irrégulier, possède deux articulations spéculaires qui la lient aux os temporaux (ATM), de forme et de fonction complexes, du fait de leur capacité à assurer des mouvements de rotation et de translation à la présence de disques interarticulaires ( sur lequel s'adaptent les têtes supérieures de la mu scoli ptérygoïde externe).Cela garantit que la mandibule peut se déplacer dans les différents plans de l'espace et dans des directions pratiquement infinies, bien que pour des étirements modestes. La riche musculature masticatrice, insérée des deux côtés de la mandibule, est également obligée de participer à n'importe quelle position ou mouvement mandibulaire en même temps. La fonction musculaire est essentiellement assurée par des muscles élévateurs robustes, par des muscles abaisseurs moins puissants, car ils sont assistés par la force de gravité et par d'autres muscles qui provoquent des mouvements de protrusion-rétrusion. De nombreux muscles cervicaux coopèrent avec les muscles masticateurs, notamment le trapèze et le sternocléidomastoïdien auxquels est confié le mouvement de la tête sur le cou, qui déterminent par conséquent la position de la mâchoire supérieure.

De tous les mouvements que la mandibule peut effectuer, celui qui provoque le plus de contact possible entre les deux arcades dentaires mérite une attention particulière. à la fin de chaque cycle masticatoire et généralement au début de chaque acte de déglutition, soit jusqu'à 2000 fois environ en 24 heures. Chaque composant de l'appareil stomatognathique, les muscles, les articulations, les muqueuses et surtout les ligaments alvéolo-dentaires qui entourent chaque racine sont richement innervés par des mécanorécepteurs.Par conséquent, tout contact entre les arcades dentaires en intercuspidation maximale provoque un apport proprioceptif qui influence le tonus et la posture musculaire, qui en termes de nombre et de concentration de récepteurs, sont peut-être inégalés dans aucune autre zone de l'organisme.L'occlusion dentaire, conditionnée par le nombre, la forme et la position des dents, est donc impliquée dans la posture de la tête pour l'atteinte des muscles cervicaux. De nos jours, la position d'occlusion est considérée comme physiologique, ce qui est obtenu grâce à une contraction isotonique et équilibrée des muscles compétents. A chaque fois que cet équilibre ne pourra être atteint pour différentes raisons, mais surtout liées à la situation des arcades dentaires, il y aura une occlusion « adaptée » qui doit être considérée comme pathologique.
Physiopathologie de la douleur musculo-squelettique
Les progrès de la connaissance clinique de la douleur musculaire, avec ses manifestations syndromiques complexes, au cours des vingt dernières années, ont été acquis grâce à de nombreux chercheurs, parmi lesquels la personnalité de Janet Travell a excellé, dont les études ont ouvert un nouveau chapitre fondamental du diagnostic d'une des souffrances les plus répandues.
La douleur, définie myofasciale car impliquant les muscles squelettiques et ses fascias et aponévrose, s'installe de préférence dans les muscles avec un engagement postural plus important, à la fois pour des causes à action chronique (comme l'engagement à une adaptation posturale forcée), et pour des causes traumatiques aiguës ( comme par exemple le "coup du lapin"). La pathogenèse de ma douleur fasciale est liée à une lésion microtraumatique des structures musculaires fines, sarcolemme et réticulum endoplasmique, qui déterminerait une augmentation du calcium libre endocellulaire, induisant un raccourcissement stable de les sarcomères entraînant l'établissement d'un état de crise de l'équilibre énergétique musculaire et une incapacité à recapturer le calcium.Il a été établi que, lorsque la contracture se produit dans les zones d'un muscle où se trouvent les plaques motrices, il y a un état de dysfonctionnement de certaines plaques qui, en produisant de l'acétylcholine en excès par rapport à la capacité d'hydrolyse de la cholinestérase, elle conduirait à une série de cercles vicieux avec une augmentation de la contracture, des spasmes capillaires, une diminution de l'apport métabolique, mais aussi la libération de substances à effet sensibilisant tant sur les terminaisons nerveuses sensibles que sur les terminaisons végétatives présentes dans la zone. Le cercle vicieux qui vient d'être décrit déterminerait l'origine des points de déclenchement myofasciaux (TrP).Un TrP (Fig. 2) est un nodule hyperexcitable placé dans une bande de tissu musculaire tendu et donc disponible à la palpation, qui s'il est stimulé donne lieu à une réponse douloureuse locale intense, parfois accompagnée d'autres phénomènes comme une réponse de contraction locale, douleur référée dans une zone bien définie et constante pour chaque point déclencheur et des réponses neurovégétatives et proprioceptives altérées. Le symptôme le plus caractéristique est la douleur projetée ; la pathogenèse de cette allodynie particulière n'est pas entièrement claire; d'autre part, on sait qu'il se manifeste toujours dans un endroit spécifique typique du point déclencheur qui l'a généré. Le site TrP étant constant dans les corps musculaires, du fait de leur interdépendance avec le locus des plaques motrices (Pr "central") ou avec les insertions muscle-tendon (Pr "attaque"), il a été possible de créer une carte de les zones de référence de la douleur, en tenant compte du fait que les points déclencheurs provenant de différents muscles peuvent également avoir en commun le site de la douleur référée.

Etiopathogenèse et Clinique des troubles cranio-mandibulaires
Le mouvement mandibulaire qui détermine la rencontre des arcades dentaires en occlusion, compte tenu de son itération continue, nécessite une action musculaire rapide et directe. Par conséquent, la position de départ de la mandibule, communément appelée position de repos, doit être dans des conditions telles qu'il effectue ce mouvement instantanément. La position de repos idéale est celle dans laquelle la musculature est également dans un état de repos, ne gardant que le tonus de base comme seule activité contractile. L'occlusion physiologique peut être réalisée à partir de la position de repos physiologique, qui dépend totalement de l'efficacité de la dentition.Lorsque ces conditions n'existent pas, les muscles masticateurs et cervicaux doivent intervenir pour créer une accommodation préventive de la position de repos mandibulaire afin de rendre la mouvement direct et prêt.L'accommodation s'effectue par une série de contractions musculaires qui annulent en réalité la situation de repos musculaire, au lieu d'établir une harmonie de différentes têtes musculaires, comme on peut le vérifier au moyen de l'électromyographie.
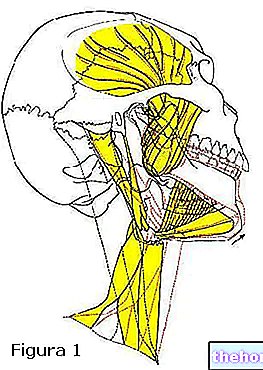
Les noxae qui peuvent altérer l'occlusion sont nombreux et peuvent agir à tout âge de la vie ; ils sont liés à des perturbations du développement des os maxillaires, à des perturbations de l'éruption et de l'alignement ultérieur des dents, aux maladies dentaires qui déterminent les dommages organiques voire la perte de la dent malade et enfin à des causes liées aux thérapies dentaires, lorsqu'elles ne parviennent pas à restaurer des conditions morphologiques et fonctionnelles satisfaisantes des arcades dentaires. La conséquence inévitable de ces noxae est l'occlusion logée dans une position posturale forcée et aujourd'hui considérée à juste titre comme pathologique.L'altération occlusale engendre une affection appelée « Trouble cranio-mandibulaire » qui peut être caractérisée par différents tableaux cliniques. Le tableau clinique, dans la plupart des cas, est dépourvu de symptômes mais ne contient que des signes objectifs qui expriment un état d'équilibre précaire. Quand et si cet équilibre venait à se rompre, des céphalées de tension et des douleurs cervicales surviennent, expression dans la région de la tête et du cou du syndrome de la douleur myofasciale. Enfin, il existe des tableaux cliniques compliqués par des phénomènes pathologiques concomitants affectant l'ATM, forcés par la luxation forcée de la mandibule, qui génèrent des bruits et des gênes articulaires de nature et de degré divers avec ou sans manifestations douloureuses. Pour mieux comprendre la pathogenèse myogénique possible de ces céphalées, il est utile de consulter la carte des zones de référence de la douleur provoquée par les principaux points déclencheurs, inspirée du texte de Travell et Simons (Fig. 3).

Tableau 1 - Corrélation entre les céphalées et le point déclencheur myofascial, selon les critères de la Classification of Headaches, Cranial Neuralgia and Facial Pain of the International Headache Society.
Procédures de diagnostic
Les procédures de diagnostic sont divisées en deux phases distinctes. La première, confiée aux critères de la sémiotique clinique, vise à rechercher l'existence de troubles affectant le système stomatognathique qui justifient l'orientation diagnostique vers l'affection de Trouble Crânio-mandibulaire et vers l'éventuelle interdépendance entre celle-ci et la céphalée, en recourant à la « anamnèse », à l'examen des radiogrammes (généralement une orthopantomographie des arcades dentaires suffit, accompagnée, si nécessaire, de radiogrammes des articulations temporo-mandibulaires), puis à « l'examen objectif. Cela nécessite à son tour un « examen minutieux de la posture de la tête sur le cou en vues antéro-postérieure et latérale et de la forme du visage, le patient étant debout ; un » examen minutieux de la cavité buccale dans les différents composants, dents unitaires et arcades dentaires muqueuses des lèvres et des joues, langue, voûte palatine, etc. Les mouvements de la mandibule en ouverture, fermeture, saillie et latéralité seront ensuite examinés ; les vibrations et les bruits articulaires associés aux mouvements doivent être détectés ainsi que l'existence éventuelle de douleurs articulaires palpatoires. L'ensemble des signes et symptômes spécifiques recueillis avec ces manœuvres est généralement suffisant pour orienter vers un diagnostic d'occlusion pathologique et de pathologie myofasciale associée. Dans ce cas, il est nécessaire de rechercher l'occlusion idéale, ce qui est indispensable pour planifier le traitement.Pour cela, il faut utiliser la deuxième phase de diagnostic, qui est instrumentale informatisée :
- Électromyographie de surface ;
- Kinésiographie (balayage des mouvements mandibulaires);
- Sonographie pour enregistrer les vibrations et les bruits produits par les articulations de la mâchoire en mouvement ;
- DIZAINES. basse fréquence;
Le test diagnostique débute par l'enregistrement électromyographique au repos du temporal, du masséter, du digastrique et du sternocléidomastoïdien, détectés à l'insertion mastoïdienne.D'autres couples musculaires, comme le trapèze, peuvent également être enregistrés.

Le test est répété après l'application de T.E.N.S pendant environ une heure. La comparaison entre les traces avant et après l'induction de relaxation fournit des données d'un grand intérêt.En résumé, une diminution généralisée des valeurs signifie l'existence d'un état hypertonique, avec un retour à une situation temporaire de normalité induite par l'effet de la TENS sur les muscles masticateurs, ce qui permet à son tour une position spatiale détendue de la mâchoire, définie comme la "position physiologique de repos"
idéal pour enregistrer le mouvement physiologique vers le meilleur contact occlusal. Il est possible, à l'aide du scanner mandibulaire, d'observer le mouvement dans les trois plans de l'espace, en documentant les trajectoires du chemin suivi.En cas d'occlusion pathologique, des altérations quantitatives et qualitatives de ce chemin seront observées et il sera possible, en introduisant un matériau d'enregistrement particulier entre les dents, retrouver la position d'occlusion physiologique représentée par un trajet idéal en situation d'équilibre des valeurs électromyographiques.
Adresses thérapeutiques
La thérapie de l'occlusion pathologique et des symptômes associés est de type orthopédique et consiste en l'application d'un dispositif intra-oral en résine, de préférence appliqué à l'arcade inférieure et construit selon les résultats obtenus à l'examen instrumental (Fig. 4).

Tableau 1