Définition de chéloïde
Les chéloïdes sont des lésions cicatricielles qui se développent au-delà des limites d'une lésion cutanée : par conséquent, à partir d'une abrasion ou d'une plaie, les chéloïdes développent une cicatrice beaucoup plus large et plus étendue que les dommages d'origine.

- Rappelons brièvement que le tissu de granulation richement vascularisé est constitué de fibroblastes, de myofibroblastes, de cellules inflammatoires et de MEC (matrice extracellulaire).
La présence d'une ou plusieurs chéloïdes sur la peau est souvent observée chez des sujets âgés de 10 à 30 ans, notamment chez les hispaniques, les afro-américains et les asiatiques. Malgré cela, les chéloïdes peuvent encore apparaître chez les personnes de tous âges.
Curiosité
Le curieux terme « chéloïde » dérive d'un mot grec χηλή (chele) qui, en italien, signifie littéralement « semblable aux pinces du crabe » : en effet, la consistance solide et l'aspect spongieux de la chéloïde forment une sorte de relief motif sur la peau, semblable aux pinces d'un crabe.
Causes
Nous avons vu que les chéloïdes sont des cicatrices étendues et anormales qui peuvent provenir d'un traumatisme cutané initial. Les principaux accusés sont sans aucun doute les perçages d'oreilles, les lésions d'acné très sévères, les brûlures et les plaies chirurgicales (des exemples typiques sont les chéloïdes qui surviennent en correspondance avec une césarienne). Parfois, certaines chéloïdes peuvent également être observées dans les zones qui ont été vaccinées ou où de petits les cicatrices de la varicelle sont restées.
Saviez-vous que...
Le terme « chéloïdose » est utilisé pour remplacer « chéloïde » lorsque de telles lésions cicatricielles sont très nombreuses (par exemple les cicatrices chéloïdes causées par « l'acné sévère) ou récidivantes.
Mais pourquoi et comment se forme une chéloïde ?
Ces lésions cicatricielles sont principalement dues à une « prolifération excessive et non régulée de fibroblastes dans le derme profond, qui produisent des quantités anormales de collagène : la surproduction de collagène, à son tour, donne une consistance solide à la cicatrice.
Facteurs de risque
Avec les mêmes blessures et traumatismes, certaines personnes développent des chéloïdes plus rapidement (ou plus sensiblement). Partant de cette hypothèse, on pense que les chéloïdes peuvent être influencées par certains facteurs de risque, énumérés ci-dessous :
- Acné sévère
- Altération de la fonction immunitaire du sujet
- Réponse anormale à une lésion cutanée
- Carence ou excès d'hormone mélanotrope, utilisée pour la synthèse et la distribution des granules de mélanine dans les mélanocytes
- Dysfonctionnements de la matrice extracellulaire qui contrôle l'activité du facteur de croissance
- Familiarité
- Folliculite de la barbe et de la nuque
- Vaisseaux sanguins trop petits. En se bloquant, les petits canaux sanguins sont incapables d'échanger efficacement l'oxygène ; par conséquent, suite à une lésion traumatique de la peau, il favorise la formation de chéloïdes.
Signes et symptômes
Le plus grand dommage lié à la présence de chéloïdes est donné par leur apparence : en effet, de nombreux patients ont recours à un traitement pharmacologique/alternatif pour effacer les lésions, craignant qu'elles ne défigurent plus ou moins clairement leur image. En plus d'être clairement inesthétiques, les chéloïdes peuvent provoquer une gêne, des démangeaisons, une sensibilité au toucher ou une hypersensibilité de la peau où elles se développent.
La plupart des lésions chéloïdes se développent irrégulièrement pendant des semaines ou des mois; dans certains cas, la croissance peut se poursuivre pendant de nombreuses années. En fin de développement, la chéloïde se stabilise sans toutefois régresser spontanément : la disparition naturelle de ces lésions est un événement assez improbable.
Comment ils se présentent
Au stade initial, la chéloïde ressemble à une simple cicatrice surélevée : la lésion a une surface lisse, glabre (sans poils) et translucide. A ce stade, les lésions chéloïdes ont une couleur rouge foncé car elles sont extrêmement vascularisées.
Par la suite, la cicatrice commence à s'étendre et à se révéler, dépassant nettement les limites de la lésion initiale : maintenant, la chéloïde prend une couleur rosée et sa consistance devient de plus en plus épaisse et caoutchouteuse.
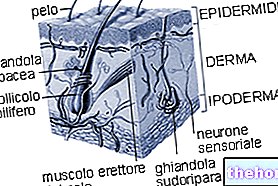
En surface, la chéloïde n'a pas de follicules pileux ni de glandes sudoripares.
Bien que les chéloïdes puissent apparaître dans n'importe quelle zone de la peau affectée par des ecchymoses ou des plaies, certaines zones du corps semblent être plus sensibles. En effet, les lésions chéloïdes sont le plus souvent observées dans la région deltoïde (épaule), au niveau du sternum et dans le haut du dos. Les lobes des oreilles et la nuque sont également des cibles courantes pour les chéloïdes.