Les symptômes sont similaires à ceux générés par d'autres affections qui évoluent vers une sciatique, comme une hernie discale ; cependant, le syndrome piriforme ne fait PAS référence à des problèmes de racines nerveuses vertébrales et/ou à la compression d'un disque intervertébral.
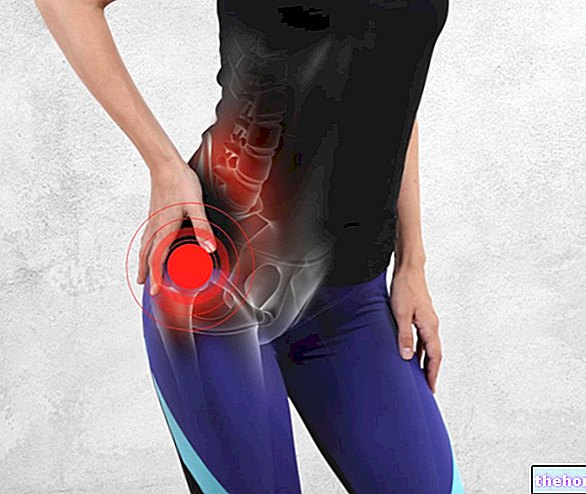
L'atteinte du nerf sciatique, en effet, survient un peu plus loin de son origine, précisément au niveau de la fesse, où il se coince en raison d'altérations du muscle piriforme, ce qui peut provoquer une douleur souvent perçue comme un picotement ou une sensation. d'engourdissement qui affecte la partie inférieure du corps et court le long de la jambe, irradiant de la fesse au pied.
La douleur peut s'aggraver pendant les activités quotidiennes telles que monter les escaliers, marcher, courir ou après s'être assis pendant de longues périodes. Le syndrome du piriforme est souvent confondu avec un problème de disque lombaire, car les symptômes sont similaires à une irritation de la racine du nerf sciatique.
Le syndrome du piriforme peut être causé par plusieurs causes, notamment des modifications anatomiques de la relation muscle-nerf ou un traumatisme de la région fessière, comme un accident de voiture ou une chute.
Il n'y a pas de test immédiat pour poser un diagnostic. La condition est principalement définie sur la base des symptômes que le patient présente et sur l'examen physique, après exclusion d'autres causes possibles.
En général, l'approche thérapeutique de la maladie commence par des exercices physiques et des étirements, qui permettent la rééducation du mouvement.La plupart des traitements visent à réduire la pression exercée par le muscle piriforme sur le nerf sciatique.
Pour contrôler la douleur et l'inflammation locales, des médicaments analgésiques et anti-inflammatoires peuvent être prescrits ; une injection locale de corticoïdes peut apporter un soulagement temporaire. Dans certains cas, la chirurgie est recommandée.
.
Le trouble provoque généralement des spasmes et des douleurs dans la fesse, mais peut également s'étendre au nerf sciatique voisin, provoquant un engourdissement, une faiblesse et des picotements à l'arrière de la jambe et dans le pied (semblable à une douleur sciatique causée par une hernie discale).
En général, les affections de ce type sont appelées NEUROPATHIES ENTRAPPANTES.

Muscle piriforme : caractéristiques et fonctions
Le piriforme est un petit muscle de forme triangulaire situé profondément dans la fesse, derrière le grand fessier.
Le muscle piriforme :
- Il provient de la surface interne du sacrum et est inséré dans le fémur homolatéral;
- Il est classé parmi les muscles externes de la hanche (groupe des rotateurs externes de la hanche) ;
- Il est important d'aider à la rotation externe/interne de la hanche et de tourner la jambe et le pied vers l'extérieur. En général, ce muscle est important dans le mouvement de la partie inférieure du corps, car il stabilise l'articulation de la hanche et, en se contractant, fait tourner le fémur vers l'extérieur et vous permet de marcher, de déplacer votre poids d'un pied à l'autre et de maintenir l'équilibre de la hanche ;
- Le nerf sciatique passe sous le muscle piriforme, avec lequel il est en contact étroit.
Les causes exactes du syndrome piriforme sont inconnues, mais certaines hypothèses incluent :
- Spasme du muscle piriforme ou d'une structure adjacente, en réponse à un événement traumatique ou à un effort excessif ;
- Anomalies musculaires avec hypertrophie ;
- Anomalies nerveuses (partielles ou totales);
- Hyperlordose lombaire ;
- Fibrose (due à un traumatisme);
- Pseudo-anévrismes de l'artère fessière inférieure ;
- Activité physique excessive.
Chacune de ces causes, ou une combinaison d'entre elles, peut affecter le muscle piriforme (provoquant des douleurs dans les fesses) et le nerf sciatique adjacent (provoquant des douleurs, des picotements ou un engourdissement à l'arrière de la cuisse, du mollet ou du pied).
Les blessures d'abus à l'origine du syndrome piriforme peuvent résulter d'activités réalisées en position assise qui impliquent une utilisation intensive des jambes, comme l'aviron ou le vélo.
Le syndrome du piriforme peut également être causé par « une pronation excessive du pied, où le muscle piriforme se contracte à plusieurs reprises, pour un mécanisme compensatoire, à chaque pas.
Le résultat du spasme du muscle piriforme peut affecter non seulement le nerf sciatique, mais aussi le nerf pudendal, qui contrôle les muscles des viscères et de la vessie. Les symptômes de compression du nerf pudendal comprennent un engourdissement et des picotements dans la région de l'aine et peuvent entraîner une incontinence urinaire et fécale.
picotements ou engourdissements dans le bas du dos, le long de l'arrière de la cuisse, du mollet et du pied (semblable à une sciatique);Quelles activités peuvent exacerber la douleur ?
Les symptômes du syndrome piriforme s'aggravent souvent lors d'activités physiques impliquant le muscle piriforme ou après une position assise prolongée, alors qu'ils peuvent s'améliorer avec le repos en décubitus dorsal.
Pour en savoir plus : Symptômes Syndrome du piriforme : c'est une version sophistiquée de la résonance magnétique et permet de mettre en évidence l'inflammation et les effets sur les nerfs impliqués.Certains spécialistes pensent que le critère de diagnostic le plus important est l'exclusion de la sciatique résultant d'une compression/irritation des racines nerveuses rachidiennes.Le syndrome du piriforme n'implique pas de hernie discale.
Cependant, le diagnostic du syndrome piriforme est basé sur un examen des antécédents médicaux du patient, un examen physique et certains tests de diagnostic.
Anamnèse
Dans le processus de diagnostic, l'anamnèse comprend un examen approfondi des symptômes signalés par le patient, en étudiant spécifiquement :
- Quelles positions ou activités soulagent ou aggravent la douleur
- La durée des événements ;
- L'association possible de symptômes avec une blessure récente et antérieure.
Examen physique
Le syndrome du piriforme est souvent défini par une série de tests de diagnostic qui excluent d'autres affections pouvant provoquer des symptômes similaires chez le patient, telles qu'une hernie discale lombaire ou un dysfonctionnement sacro-iliaque.
La visite comprend un examen de la hanche et des jambes pour :
- Évaluer si le mouvement provoque une exacerbation de la douleur dans le dos ou les membres inférieurs ;
- Mesurer la douleur locale et la force musculaire.
Généralement, le mouvement de la hanche et la rotation forcée de la cuisse en extension provoquent des douleurs, tandis qu'une palpation minutieuse et profonde permet de détecter un spasme du muscle piriforme.

Diagnostic pour les images
Les tests d'imagerie traditionnels ne peuvent pas diagnostiquer le syndrome piriforme.
Cependant, des investigations telles que la tomodensitométrie (TDM) et l'imagerie par résonance magnétique (IRM) peuvent être menées pour :
- Écarter d'autres conditions responsables de symptômes similaires ;
- Détectez si le nerf sciatique est comprimé à cause d'autres causes.
Une "injection d'anesthésique, avec ou sans corticostéroïdes, peut aider à confirmer si le muscle piriforme est à l'origine des symptômes".
®), qui peut soulager la raideur musculaire et la compression du nerf sciatique.Une approche globale de la gestion du syndrome piriforme peut inclure une combinaison des traitements suivants.
Exercices, étirements et massages
Un traitement efficace comprend l'étirement et le renforcement des groupes musculaires touchés par le syndrome du piriforme (moyen fessier, muscles adducteurs et extenseurs de la hanche, etc.). Des exercices qui impliquent des mouvements pour étirer le muscle piriforme et diminuer les spasmes peuvent soulager les symptômes douloureux le long du nerf sciatique et réhabiliter le patient en quelques jours.
La massothérapie, pratiquée par un expert, peut aider à guérir le syndrome du piriforme en augmentant le flux sanguin dans la région et en réduisant les spasmes musculaires.

Compresses froides et chaudes
Lorsque la douleur survient, il est utile de commencer par appliquer une compresse froide sur la zone douloureuse plusieurs fois par jour, pendant environ 15 minutes à la fois. Répétez si nécessaire toutes les 2 à 4 heures, en continuant jusqu'à ce que cela vous profite, même pendant quelques jours.
Parfois, il peut être plus utile de masser doucement la zone avec un glaçon, surtout si des activités spécifiques provoquent une augmentation de la douleur (si la glace est placée directement en contact avec la peau, limitez l'application à 8-10 minutes pour éviter les brûlures par le froid) .
La compresse froide aide à soulager l'inflammation et les tensions musculaires liées au syndrome du piriforme, pour un effet analgésique naturel.
Une fois la douleur aiguë soulagée, il est bon d'essayer de détendre les muscles contractés : dans ce cas, la chaleur (comme une bouillotte) peut être utile.
Certaines personnes atteintes du syndrome piriforme trouvent utile d'alterner entre les compresses froides et chaudes.
Médicaments
Les anti-inflammatoires non stéroïdiens (AINS), tels que l'ibuprofène ou le naproxène, aident à soulager la douleur pendant la phase aiguë du syndrome piriforme et aident à réduire l'inflammation.
Si la douleur n'a pas tendance à s'améliorer, les médecins peuvent injecter un corticostéroïde directement dans le muscle piriforme pour réduire les spasmes musculaires.
Le but d'une "injection locale de médicaments est de diminuer la douleur aiguë pour permettre des progrès en physiothérapie".
Pour un spasme persistant du muscle piriforme, résistant aux traitements antalgiques et anti-inflammatoires, il peut être utile de recourir à une injection de toxine botulique, pour aider le muscle à se détendre et aider à réduire la pression sur le nerf sciatique.
Électrothérapie pour le syndrome du piriforme
La stimulation nerveuse électrique transcutanée (TENS) peut aider à bloquer la douleur et à réduire les spasmes musculaires associés au syndrome piriforme.





-cloruro.jpg)