Généralité
La thyroglobuline (Tg) est le constituant principal du colloïde, contenu dans les follicules thyroïdiens, plus précisément une glycoprotéine iodée (contenant de l'iode) produite par les cellules thyroïdiennes (thyrocytes).

Si nécessaire, la thyroglobuline est réabsorbée par le colloïde, puis elle est décomposée pour donner naissance à la triiodothyronine (T3) et à la thyroxine (T4).
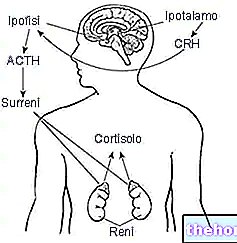
La production de ces hormones thyroïdiennes et leur libération dans la circulation sanguine sont stimulées par l'hormone hypophysaire TSH (hormone stimulant la thyroïde).
Le dosage de la thyroglobuline dans le sang est principalement utilisé comme marqueur tumoral, pour évaluer l'efficacité du traitement du cancer de la thyroïde et pour surveiller les rechutes.
Qu'est-ce que c'est ça
La thyroglobuline (Tg) est la molécule de glycoprotéine précurseur des hormones thyroïdiennes T3 et T4.
La glande thyroïde est organisée en follicules très petits et très serrés, à tel point qu'à l'âge adulte il y en a environ 3 millions. En dehors de ces structures circulaires, on trouve un épithélium folliculaire monostratifié cubique, tandis que dans la partie interne se trouve un liquide gélatineux et jaunâtre, le colloïde, constitué principalement de thyroglobuline.
La thyroglobuline est synthétisée par les cellules épithéliales (thyrocytes) du follicule, elles-mêmes entourées d'un réseau capillaire dense, ce qui fait de la thyroïde l'une des structures les plus vascularisées de l'organisme.C'est par la circulation sanguine que l'iode atteint le follicule ; en effet indispensable à la synthèse des hormones thyroïdiennes, qui part de l'ionisation de la thyroglobuline par l'enzyme iodase (appelée aussi TPO ou iodure peroxydase).
A l'intérieur de la molécule de thyroglobuline (qui contient 70 tyrosines), grâce à l'intervention de l'iodase, des résidus de tyrosine à un ou deux atomes d'iode peuvent se former, respectivement appelés MIT ou 3-monoiodotyrosine et DIT ou 3,5-diiodotyrosine.

Une fois produites, T3 et T4 ne sont pas libres, mais restent partie intégrante du peptide de thyroglobuline plus complexe.
La TSH ou hormone thyréotrope, d'origine hypophysaire, est le principal facteur de contrôle, à la fois de la synthèse de la thyroglobuline et de la libération des hormones thyroïdiennes dans la circulation. Ce dernier processus se déroule grâce à un mécanisme cellulaire complexe ; les thyrocytes épithéliaux, en fait, la thyroglobuline phagocytaire, qui à l'intérieur des vésicules (phagosomes) subit l'action dégradante des enzymes lysosomales : le lien entre la thyroglobuline et les hormones thyroïdiennes est rompu et la même glycoprotéine dégradée. Ainsi, d'une part les hormones thyroïdiennes sont libérées dans la circulation sanguine, tandis que d'autre part ce qui reste de la thyroglobuline est recyclé à l'intérieur de la même cellule, puis utilisé pour la synthèse de nouvelles protéines et hormones thyroïdiennes.
Parce qu'il est mesuré
Le dosage de la thyroglobuline est utile pour surveiller le traitement du cancer de la thyroïde. Souvent, ce test est prescrit à intervalles réguliers après la chirurgie pour détecter une récidive ou une propagation du processus néoplasique.
La thyroglobuline n'est pas synthétisée par toutes les tumeurs thyroïdiennes, mais dans les formes les plus courantes (telles que l'adénocarcinome papillaire et folliculaire) une augmentation de ses concentrations sanguines est fréquemment observée.

En présence de certains troubles thyroïdiens, un test de thyroglobuline peut être demandé avec d'autres tests impliquant la glande.