La conjonctive aussi
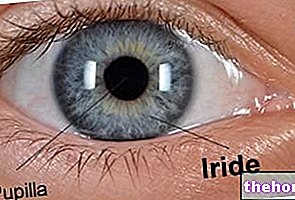
La conjonctive est la fine membrane muqueuse qui recouvre la surface antérieure du globe oculaire (à l'exception de la cornée) et la surface interne des paupières.
Sa fonction principale est de protéger l'œil, grâce au revêtement qu'il procure, des corps étrangers et des infections.De plus, cette structure oculaire anatomique contribue au maintien du film lacrymal et facilite le glissement des deux surfaces conjonctivales opposées, évitant ainsi les frottements. les phases clignotantes.
La conjonctive peut être le siège de nombreux processus pathologiques : inflammation (conjonctivite), malformations congénitales, tumeurs bénignes ou malignes, modifications dystrophiques et maladies dégénératives. De plus, des affections générales de l'organisme de divers types, telles que des maladies infectieuses, des réactions allergiques et des troubles métaboliques, affectent la conjonctive.

Structure
La conjonctive est une membrane muqueuse, presque totalement transparente, bien vascularisée et abondamment innervée par des filaments trijumaux (appelés nerfs ciliaires).
Du point de vue histologique, la tunique conjonctivale est constituée de cellules épithéliales (épithélium colonnaire et squameux), disposées en 2 à 5 couches, et de stroma (tissu conjonctif). De plus, il existe un système glandulaire, constitué principalement de cellules caliciformes qui contiennent des granules de mucine et assurent la production de la couche muqueuse du film lacrymal.
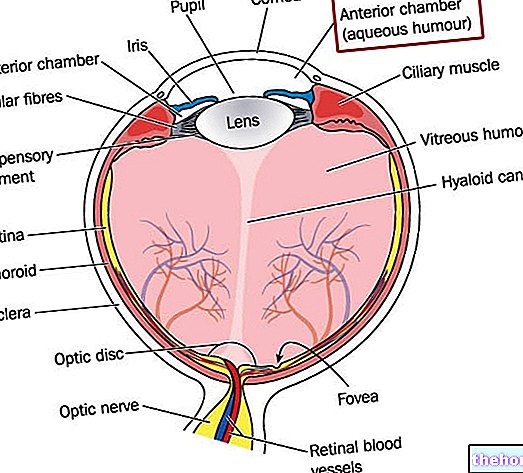
La conjonctive peut être divisée en 3 parties anatomiques :
- Conjonctive de la paupière (ou tarse) : constituée d'un épithélium cylindrique, c'est une membrane fine, transparente, rouge ou rose. Suivant la peau, la tunique conjonctivale débute au bord libre des paupières, puis recouvre la face postérieure des tarses, sur laquelle elle adhère fortement.
- Conjonctive bulbaire (ou sclérale) : c'est la partie de la tunique conjonctivale qui s'applique sur le globe oculaire et recouvre la surface antérieure de la sclère, à l'exception de la partie cornéenne. Constituée d'un épithélium pavage, la conjonctive bulbaire repose faiblement sur une lamina propria conjonctive lâche. La tunique conjonctivale bulbaire est lisse, très fine et si transparente que l'on peut voir la couleur blanche des vaisseaux sclérosés et antérieurs conjonctivals et ciliaires. En position médiale, la conjonctive tarsienne reçoit donc les points lacrymaux supérieur et inférieur, qui représentent le début des canaux lacrymaux.
- Conjonctive des fornix : au niveau de l'espace entre les paupières et le globe oculaire, la membrane conjonctivale se replie et recouvre les fornix supérieur et inférieur, laissant la liberté de mouvoir le bulbe.
Sac conjonctival
Dans son ensemble, la conjonctive forme une sorte de "poche", qui résulte du repliement de la membrane bulbaire (qui tapisse l'œil) et de la membrane palpébrale (adhérant à la partie interne des paupières).Le sac conjonctival est fermé lorsque les bords libres des paupières entrent en contact lors du clignement, tout en communiquant avec l'extérieur lorsque le sillon palpébral est ouvert.
Caroncule lacrymale et pli semi-lunaire de la conjonctive
Au coin interne de la fissure palpébrale, il existe deux formations qui représentent des rudiments de structures embryonnaires : le pli lunaire et la caroncule lacrymale.
Le pli semi-lunaire est un pli vertical de la conjonctive bulbaire dont le bord libre est concave. Il s'étend du fornix supérieur au fornix inférieur de la conjonctive, mais n'est visible que dans sa partie médiane, étant en grande partie caché par les paupières.
La caroncule lacrymale est, d'autre part, une petite excroissance muqueuse rose, arrondie et surélevée, placée entre les parties lacrymales des marges de la paupière ; il contient un stroma conjonctif dense, traversé par quelques faisceaux de cellules musculaires lisses et striées. La caroncule lacrymale a des follicules pileux avec des poils rudimentaires et des glandes sébacées attachées. Il contient également des glandes lacrymales accessoires.
Remarque : chez l'homme, le pli lunaire au coin de l'œil est considéré comme un petit vestige de la membrane nictitante, c'est-à-dire la « troisième paupière » que l'on observe chez d'autres animaux, comme les oiseaux et les reptiles.
Les fonctions
La conjonctive a pour fonction principale de protéger la surface antérieure de l'œil.
De plus, il facilite le glissement des paupières dans les phases de clignement et permet au globe oculaire de bouger, sans frottement au niveau de ses surfaces, grâce à la sécrétion de la composante mucine du film lacrymal (sorte de mucus visqueux qui protège la cornée et permet aux larmes aqueuses prééminentes de se stratifier).
La conjonctive contient, en effet, des glandes séreuses, mucipares (ou cellules caliciformes sécrétant du mucus) et des glandes lacrymales accessoires (de Krause et de Ciaccio). Ces structures versent leur sécrétion à l'intérieur du sac conjonctival, aidant ainsi à garder la surface oculaire humide, propre et intacte.
En plus de la protection physique et biologique des larmes, la conjonctive possède un système de défense immunitaire médié par des éléments lymphatiques, principalement situés dans la partie tarsienne (follicules lymphatiques). Du fait de son anatomie particulière, en effet, le tissu conjonctival est particulièrement exposé aux agents externes, tels que la poussière, le pollen et les bactéries.
Remarque : la muqueuse conjonctivale répond à des stimuli de nature différente, qui modifient son aspect.Ces réactions, par exemple, peuvent provoquer une rougeur due à la dilatation des vaisseaux sanguins de la conjonctive (hyperhémie) ou provoquer un tableau plus grave avec écoulement abondant, douleur, sensation de corps étranger et larmoiement, parfois associés à une tuméfaction œdémateuse (chémosis).
Conjonctivite
La conjonctivite est une « inflammation de la surface conjonctivale. C'est une pathologie fréquente, qui peut se manifester sous une forme aiguë ou chronique.
Les causes peuvent être diverses, mais les plus fréquentes sont les suivantes :
- Infections oculaires (dues à des bactéries, virus, champignons ou parasites);
- Allergies saisonnières ou pérennes (hypersensibilité au pollen, aux cosmétiques, aux acariens ou aux poils d'animaux) ;
- Irritation intense due aux corps étrangers et aux agents physico-chimiques (causée par les médicaments, la chaleur, le vent, la poussière et les polluants atmosphériques, les acides, les alcalis, le savon, la fumée de cigarette et les engrais, une exposition excessive au soleil ou à d'autres formes de rayonnement, etc.).
Les symptômes de la conjonctivite dépendent des causes, mais comprennent souvent des brûlures, des démangeaisons, des rougeurs, une photophobie, une augmentation de la formation de larmes, un gonflement des paupières et une sensation de corps étranger (une sensation d'avoir du sable dans les yeux). Dans la forme infectieuse, un écoulement catarrhal ou mucopurulent peut s'ajouter aux manifestations répertoriées (les yeux ont tendance à "coller").
Le traitement varie selon le type de conjonctivite et est établi par un ophtalmologiste.
Les formes bactériennes peuvent être guéries avec un traitement antibiotique par collyre. Dans le cas de la conjonctivite allergique, en revanche, des gouttes oculaires antihistaminiques et cortisone sont utilisées, ce qui peut être associé à l'utilisation de larmes artificielles et d'antihistaminiques systémiques.
Les formes virales souvent causées par l'adénovirus et le virus de l'herpès ont une évolution plus longue et plus difficile que la conjonctivite bactérienne. En général, des instillations fréquentes de collyre antibiotiques sont utilisées (afin de prévenir la surinfection bactérienne) et, avec prudence, des médicaments topiques à base de cortisone (pour diminuer l'hyperémie et l'œdème conjonctival).
Hémorragie sous-conjonctivale
L'hémorragie sous-conjonctivale se présente sous la forme d'une tache rouge vif, non associée à d'autres signes d'inflammation.Ces extravasations sanguines sous la conjonctive résultent d'une rupture d'une paroi capillaire et apparaissent généralement à la suite de traumatismes mineurs, de toux et d'éternuements (par exemple, au cours d'affections Dans certains cas, l'hémorragie sous-conjonctivale peut s'accompagner d'hypertension artérielle systémique, de dyscrasies sanguines et de conjonctivite virale.
Le trouble a tendance à disparaître spontanément en 15 jours environ, aucun type de traitement n'est donc nécessaire. Dans tous les cas, il est conseillé de contacter votre ophtalmologiste pour une évaluation.
Corps étranger conjonctival
La présence d'un corps étranger au niveau conjonctival provoque des symptômes unilatéraux, caractérisés par des douleurs, des difficultés à garder l'œil ouvert, une hyperémie conjonctivale, des larmoiements et une photophobie.
S'ils sont maintenus au niveau du tarse, les corps étrangers peuvent provoquer des lésions cornéennes dues au frottement continu de la paupière pendant le clignement, c'est pourquoi ils doivent être retirés le plus rapidement possible.
Dégénérescence conjonctivale
La pinguécule et le ptérygion sont des dégénérescences bénignes de la conjonctive, qui apparaissent comme des excroissances adjacentes à la cornée. Ces deux blessures provoquent des rougeurs, des irritations, des sensations de corps étranger et des brûlures.
Pinguécula
La pinguécule est une accumulation de collagène dégénéré, localisée dans le secteur conjonctival nasal et temporal.

La pinguécule peut représenter le résultat d'une inflammation de la surface oculaire suite à un traumatisme, des brûlures caustiques et des ulcérations cornéennes périphériques.
Ptérygion
Le ptérygion est une petite formation fibrovasculaire en forme de triangle causée par une croissance anormale de la conjonctive bulbaire. Cette lésion s'étend progressivement vers la cornée, jusqu'à la recouvrir. Contrairement à la pinguécule, en effet, le ptérygion possède ses propres vaisseaux.
Cette lésion se produit généralement du côté nasal de la cornée et entraîne souvent une réduction de l'acuité visuelle par induction de l'astigmatisme. En effet, le ptérygion peut déformer la surface cornéenne, modifiant le pouvoir de réfraction de l'œil.
La réduction de la vision détermine la nécessité d'enlever la lésion chirurgicalement, même si les récidives sont très fréquentes.
Les causes du ptérygion sont encore en partie inconnues, cependant l'exposition chronique à des facteurs irritatifs (notamment au soleil et au vent) augmente le risque de développer la maladie.
Pemphigoïde cicatricielle
La pemphigoïde cicatricielle est une altération caractérisée par une cicatrisation progressive et un rétrécissement bilatéral de la conjonctive.Ce processus est également associé à la néovascularisation, l'opacification et la kératinisation simultanées de la cornée.
Le mécanisme de la pemphigoïde cicatricielle est auto-immun.
Au début, la maladie se manifeste de manière similaire à une conjonctivite chronique, provoquant une hyperémie, une gêne, des démangeaisons et des sécrétions.La progression de la maladie conduit cependant à des phénomènes tels que le symblépharon (adhérence entre le tarse et la conjonctive bulbaire), le trichiasis (introflexion des cils), kératoconjonctivite sèche et kératinisation conjonctivale. Les lésions cornéennes chroniques peuvent entraîner une ulcération bactérienne secondaire et la cécité.
Le diagnostic peut être confirmé par une biopsie. Le traitement peut nécessiter une immunosuppression systémique par dapsone ou cyclophosphamide.
Tumeurs de la conjonctive
La conjonctive peut être le siège de processus néoplasiques bénins ou malins. Dans la plupart des cas, ceux-ci proviennent de l'épithélium (la couche de cellules la plus superficielle) ou des mélanocytes (présents dans l'épithélium conjonctival).
Néoplasie intraépithéliale cornéo-conjonctivale
La néoplasie intraépithéliale cornéo-conjonctivale est la tumeur de la surface oculaire la plus fréquente.Elle se manifeste par des tableaux cliniques allant de la dysplasie légère au carcinome localement invasif (provoque rarement des métastases). Typiquement, elle se présente sous la forme d'une masse conjonctivale épaissie ou blanchâtre, translucide ou gélatineuse, souvent vascularisée.
Le traitement consiste en une exérèse chirurgicale extensive, parfois associée à une cryothérapie et à une reconstruction du plan conjonctival.Le recours à une chimiothérapie topique peut également être envisagé.
Carcinome squameux
La tumeur maligne la plus courante est le carcinome épidermoïde. Cela peut provenir de zéro ou dériver d'une phase précédente in situ. Les formes initiales ressemblent à un ptérygion, tandis que les formes peu différenciées ont un aspect gélatineux et translucide. Le carcinome épidermoïde, quant à lui, prend un aspect végétatif, occupe la fissure interpalpébrale et a tendance à faire saillie vers l'extérieur.Une exérèse chirurgicale prompte et rapide, associée à la cryothérapie, la radiothérapie et la chimiothérapie topique, est généralement associée à un bon pronostic.
Tumeurs lymphoïdes
Le lymphome non hodgkinien de l'annexe oculaire est assez rare (il représente environ 8% de tous les cas extra-ganglionnaires). Généralement, ces cancers impliquent le tissu lymphoïde associé aux muqueuses, c'est ce qu'on appelle le MALT (acronyme de " tissu lymphoïde associé aux muqueuses ") et peut survenir avec l'apparition d'un gonflement des paupières ou de modifications visuelles de divers types.
Mélanome conjonctival
Dans la plupart des cas, les tumeurs pigmentées sont bénignes, mais elles doivent toujours être considérées comme d'éventuels porteurs de malignité (l'évolution est similaire à celle qui conduit à la formation d'un mélanome cutané).
Le mélanome conjonctival est une tumeur rare (il représente environ 2% des tumeurs oculaires malignes). Elle peut provenir de zéro ou résulter de la transformation de lésions pigmentées bénignes (naevus et mélanose congénitale) ou précancéreuses (mélanose primitive acquise avec atypie).
Le mélanome conjonctival peut provoquer des métastases par propagation lymphatique aux ganglions lymphatiques loco-régionaux et par voie sanguine. L'approche thérapeutique est guidée par la taille et la localisation du mélanome.Dans la plupart des cas, l'exérèse chirurgicale extensive, souvent associée à la cryothérapie, est le traitement de choix. Dans les mélanomes de grandes dimensions ou localisés dans des localisations défavorables, une chirurgie radicale est indiquée, qui consiste en l'ablation de tout le contenu orbitaire.



.jpg)