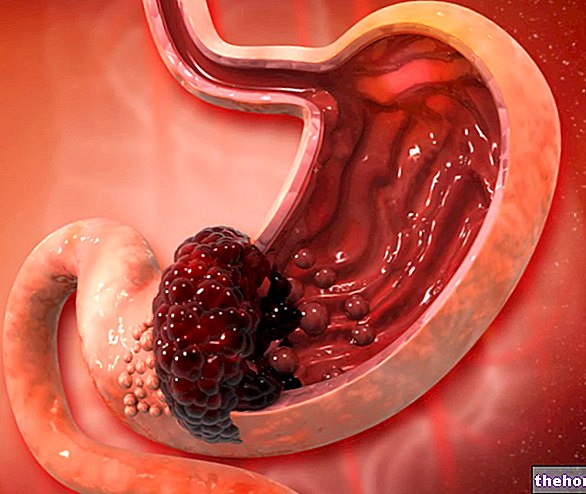
Un ulcère gastroduodénal est défini comme une pathologie grave de l'estomac et du duodénum. Moins fréquemment, elle peut toucher l'œsophage et la partie supérieure de l'intestin grêle (2% des cas).

Du point de vue étiologique, l'ulcère gastroduodénal se développe suite à l'exposition de la muqueuse aux sucs gastriques (acide chlorhydrique et pepsine) mais insuffisamment entravé par le mucus protecteur.
En pratique, l'apparition de l'ulcère est provoquée par le déséquilibre entre les facteurs agressifs et protecteurs, qui agissent sur la muqueuse gastro-duodénale.
En Occident, environ une personne sur dix a souffert, souffre ou souffrira d'un ulcère de l'estomac ou du duodénum. Les hommes (surtout d'âge moyen) sont trois fois plus touchés que les femmes, notamment au niveau du duodénum (sauf au Japon) ; parfois, l'ulcère se produit à la fois dans l'estomac et le duodénum.Il est possible que les hormones œstrogènes jouent un rôle protecteur chez les femmes fertiles.
L'apparition de l'ulcère a une base comportementale très large ; il existe également une prédisposition génétique (groupe sanguin 0). Ces dernières années, l'incidence semble avoir considérablement diminué.
Le matériel publié est destiné à permettre un accès rapide aux conseils, suggestions et remèdes généraux que les médecins et les manuels dispensent habituellement pour le traitement de l'ulcère gastroduodénal ; ces indications ne doivent en aucun cas remplacer l'avis du médecin traitant ou d'autres spécialistes de la santé du secteur qui soignent le patient.
Que faire
- La précaution la plus importante est sans aucun doute la prévention (voir Prévention ci-dessous). L'ulcère grave, même s'il est guéri, peut compromettre définitivement l'intégrité de la muqueuse (cicatrice).
- Reconnaissance des symptômes : l'identification précoce des symptômes de la maladie ulcéreuse est essentielle pour réduire l'aggravation de l'érosion. Ces symptômes sont :
- Douleurs et brûlures épigastriques :
- Dans l'ulcère gastrique, il survient une demi-heure après le repas.
- Dans "l'ulcère duodénal, il survient une heure et demie et jusqu'à trois heures après un repas. Il peut être situé à droite de la ligne abdominale.
- Parfois nausées et vomissements.
- Signes et symptômes abdominaux aigus (douleur intense, comme un coup de poignard, abdomen dur, en bois, en forme de comprimé, nausées, vomissements, transpiration, tachycardie, pouls faible et prise de position recroquevillée d'un côté) : dans ce cas, l'ulcère est souvent perforante.
- À long terme, perte de poids causée par l'anorexie et l'aversion pour la nourriture en raison de la sévérité des symptômes.
- À long terme, anémie ferriprive causée par des saignements modestes.
- Consultez votre médecin de soins primaires ou un gastro-entérologue directement pour un diagnostic spécifique. Ceci vise à exclure d'autres conditions:
- Hernie hiatale.
- Gastrite.
- Duodénite.
- L'ulcère duodénal.
- Calculose de la vésicule biliaire.
- Inflammation chronique de la vésicule biliaire.
- Cancer de l'estomac.
- Le médecin généraliste ou spécialiste réalisera des investigations endoscopiques et/ou radiologiques :
- Gastro-duodénoscopie oesophage.
- Biopsie pour la détection de la bactérie Helicobacter pylori.
- Radiographie.
- En cas de diagnostic positif, une thérapie spécifique commence :
- Adoptez une alimentation correcte (voir ci-dessous Quoi manger et quoi NE PAS manger), favorisant la digestion, limitant la distension gastrique et réduisant la sécrétion gastrique.
- Exclure tous les facteurs nocifs (voir ci-dessous Ce qu'il ne faut PAS faire).
- Thérapie pharmacologique : elle peut être de divers types (voir Traitements pharmacologiques ci-dessous).
- Chirurgie : uniquement dans les cas les plus sévères ou dans l'évolution vers le cancer.
Ce qu'il ne faut pas faire
- Mener une mauvaise hygiène de vie, sans respecter les critères de prévention.
- Ignorez les premiers symptômes.
- N'allez pas chez votre médecin pour un certain diagnostic et pour écarter d'autres maladies ou complications.
- Négliger la thérapie spécifique :
- Ne suivez pas un traitement médicamenteux.
- Ne vous faites pas opérer si votre médecin le juge essentiel.
- Suivez un régime alimentaire inapproprié.
- Fumer.
- Abus avec l'alcool.
- Exposez-vous à des contaminants environnementaux potentiellement nocifs pour l'estomac.
- Menez une vie stressante.
- Utilisez des médicaments gastro-intestinaux nocifs, en particulier à jeun et sans utiliser de protecteurs gastro-intestinaux.
Ce qu'il faut manger
L'alimentation doit être structurée de manière spécifique, pour éviter que l'ulcère ne s'aggrave. Il existe trois principes fondamentaux :
- Ne pas trop étirer l'estomac et/ou le duodénum.
- Limiter la production de sucs gastriques.
- Assurer une digestion efficace et efficiente, en évitant les longs séjours dans l'estomac.
A cet effet, il est recommandé de :
- Mangez des repas plus petits, par exemple en répartissant les calories comme suit :
- Petit déjeuner à 15% de l'énergie.
- Deux collations (snacks) à 10 % ou quatre à 5 %.
- 35% déjeuner.
- Dîner à 30%.
- Choisissez des portions modérées.
- Consommez des repas en dehors des heures de sommeil.
- Utilisez peu d'assaisonnement et principalement des huiles végétales de première pression. Nous recommandons 4 cuillères à café par jour. L'excès de graisse peut compromettre la digestibilité et l'intégrité de la barrière muqueuse.
- Privilégiez les aliments maigres et digestes :
- D'origine animale (pauvre en matière grasse et en tissu conjonctif) : poulet, dinde, lapin, muscle dégraissé de porc ou de bœuf, cabillaud, anchois, dorade, bar, corvina, courbine, filet de thon, crevettes, ricotta maigre, fromage frais léger , flocons de lait, blanc d'œuf ou au plus un entier, etc.
- D'origine végétale (pas trop de fibres) : céréales, légumineuses et dérivés, en choisissant ceux à teneur moyenne ou faible en fibres. Fruits et légumes en portions de 50-150g (même avec la peau).
- Utilisez des systèmes de cuisson qui optimisent la digestibilité :
- Faire bouillir dans l'eau.
- Bouillir sous vide.
- Vasocuisine.
- À vapeur.
- Dans une cocotte minute.
- Dans une casserole à feu doux.
- Au four (en évitant les cuissons prolongées et/ou à des températures excessives)
- Cuit.
- Aliments frais, non conservés, à consommer « naturels » ; la seule méthode de stockage à long terme recommandée est la congélation.
- Mangez des aliments à température moyenne, ni trop froids ni trop chauds.
NB : Il existe différentes formes de malnutrition liées à l'ulcère, à la pharmacothérapie et aux complications associées, dont : l'anémie ferriprive, l'anémie pernicieuse, la diminution de l'absorption du calcium et l'altération de l'absorption générale.
Ce qu'il ne faut PAS manger
- Alcool (surtout à jeun).
- Cacao, chocolat noir et menthe.
- Aliments piquants comme le piment, le poivre, le raifort, le gingembre, de grandes quantités d'oignon et d'ail crus, etc.
- Aliments et boissons contenant des xanthines (surtout à jeun) : café, thé noir, chocolat chaud, boissons énergisantes, etc.
- Gros repas et portions, surtout avant de dormir.
- Aliments très assaisonnés.
- Aliments gras, ou aliments riches en tissu conjonctif ou contenant trop de fibres : abats, morceaux gras de porc, couenne, ossobuco, saucisses, salami, saucisses de Francfort, hamburgers, saumon, anguille, poitrine de thon, poulpe, seiche, moules, palourdes, escargots , gorgonzola, fromage pecorino, mascarpone, fontina, brie, plus un jaune d'œuf à la fois, carpaccio, tartare, sushi, ragoût, ragù et similaires, soupes, viandes braisées, viande bouillie, son, légumineuses insuffisamment cuites, portions exagérées de légumes etc...
- Techniques de cuisson qui rendent les aliments difficiles à digérer :
- Mijoter.
- Faire frire dans une poêle.
- Cuisson longue au four ou sur le grill ou dans l'eau bouillante.
- Brasage.
- Aliments salés.
- Aliments conservés :
- Dans l'huile.
- En saumure.
- Au sel.
- Fumé et séché.
- Aliments et boissons qui ont tendance à être acides en portions importantes :
- Le vinaigre.
- Boissons (par exemple, cola).
- Agrumes et jus.
- Tomate et jus.
- Aliments chauds ou surgelés.
- Du lait.
- Bouillon.
- Boissons gazeuses (soda à l'orange, cola, etc.).
- Snacks et autres malbouffes.
Remèdes et remèdes naturels
- Bicarbonate de sodium (NaHCO3) : en solution aqueuse, il intervient rapidement, mais provoque quelques effets secondaires tels que : alcalinisation des urines, gonflement, hypersodémie et parfois diarrhée.
- Phytothérapie : certaines plantes sont capables d'améliorer les symptômes de l'ulcère gastroduodénal ou d'agir positivement sur le mécanisme d'action. Les plus connus sont :
- Hypericum.
- Réglisse.
- Fleur de la passion.
- Camomille.
- Consolider.
- Calendula.
- Alginates et mucilagineux qui recouvrent la muqueuse gastrique la protégeant des agents agressifs :
- Mélisse.
- Altéa.
- Mauve.
- Lichen islandais.
- Calendula.
- Teintures mères à effet cicatrisant :
- Salicaire
- Fraise.
- Ail : facilite l'éradication d'Helicobacter pylori, mais stimule la sécrétion gastrique et est contre-indiqué en cas d'ulcère.
- Huile essentielle de clou de girofle.
Traitement pharmacologique
- Antagonistes des récepteurs H2 de l'histamine : ranitidine, cimétidine (ex. Ulis, Biomag, Tagamet), famotidine et nizatidine (ex. Nizax, Cronizat, Zanizal) Pour une utilisation orale et rarement parentérale, ils inactivent la pompe à protons et réduisent la libération d'ions hydrogène.
- Antiacides (tels que l'hydroxyde d'aluminium avec l'hydroxyde de magnésium, par exemple Maalox plus).
- Inhibiteurs de la pompe à protons : bloquent la production d'histamine, de gastrine et d'acétylcholine ; en association avec des antibiotiques, ils favorisent l'élimination d'Helicobacter pylori. Par exemple:
- Pantoprazole (tel que Peptazol, Pantorc, Nolpaza, Gastroloc).
- Oméprazole (comme Antra, Nansem, Losec, Xantrazol).
- Lansoprazole (comme Pergastid, Lomevel, Lansox).
- Protecteurs de la muqueuse gastrique :
- Sucralfate (par exemple Degastril, Citogel).
- Composés du bismuth (par exemple, salicylate de bismuth).
- Analogues des prostaglandines : protègent la muqueuse en réduisant la sécrétion gastrique ; par exemple le Misoprostol (comme Cytotec).
- Antibiotiques contre Helicobacter pylori :
- Amoxicilline : par exemple Augmentin, Klavux.
- Métronidazole : par exemple Metronid, Deflamon.
- Clarithromycine.
La prévention
- Ne pas fumer.
- N'abusez pas de l'alcool, surtout à jeun.
- Suivez un régime alimentaire approprié.
- Évitez les aliments prédisposants.
- Limitez l'utilisation de certains médicaments (AINS anti-inflammatoires, stéroïdes, antibiotiques, etc.) ou au moins prenez-les l'estomac plein.
- Minimiser les niveaux de stress nerveux.
- Si possible, ne vous exposez pas à des contaminants chimiques et environnementaux nocifs (vapeurs, fumées, etc.).
- Éviter la possibilité de contagion à Helicobacter pylori, même si des études récentes suggèrent que cette bactérie est présente dans les muqueuses de tous mais ne devient pathogène que pour quelques-uns.
- Contactez le médecin avec la manifestation des premiers symptômes. De cette façon, il est possible de bloquer l'ulcère dans les premiers stades, en réduisant la gravité (lorsqu'il s'agit encore d'une simple érosion de la muqueuse superficielle), le traitement et la possibilité de complications.
Traitements médicaux
- Chirurgie : elle est adoptée lorsque les ulcères sont résistants aux thérapies médicamenteuses et comportementales, lorsqu'il existe une suspicion de forme tumorale et en cas de complications graves. Consiste en:
- Excision des branches gastriques du nerf vague, dans le but de réduire la sécrétion gastrique.
- Gastrectomie : résection d'une partie de l'estomac.