Définition
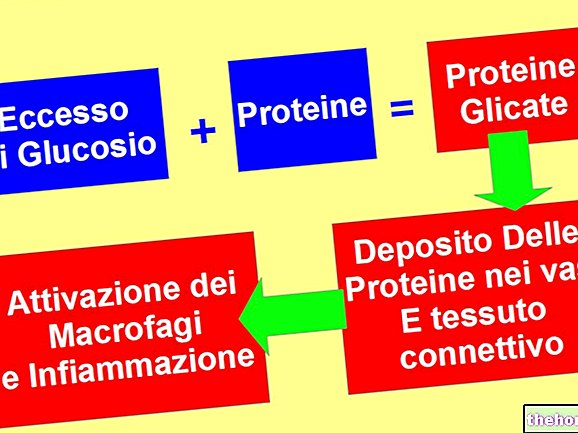
Comme le terme lui-même l'anticipe, le pied diabétique (ou pied neuropathique) représente une complication chronique redoutable du diabète : c'est un état morbide qui se développe à la suite d'une neuropathie * et d'une artériopathie *, conditions pathologiques typiques de la maladie métabolique d'origine.
* Glossaire- Neuropathie : altération du système nerveux périphérique qui se manifeste principalement par des picotements, des crampes, des troubles de la marche et une altération de la sensibilité (incapacité à percevoir la douleur, la chaleur et le froid)
- Artériopathie : état pathologique qui fait référence à des problèmes de circulation sanguine dans les artères (mauvaise circulation sanguine)
Dommages neurologiques (c'est-à-dire neuropathie diabétique) peut provoquer un engourdissement ou une perte de la capacité à ressentir la douleur et les changements de température dans les membres inférieurs. Ce qui a été dit signifie qu'un patient diabétique a tendance à ne pas remarquer la présence de coupures, blessures, brûlures, gelures etc. au niveau des pieds précisément parce que sa réponse de défense à la douleur est affaiblie.
Si, en plus de la neuropathie diabétique, s'ajoute une mauvaise circulation dans les membres inférieurs (artériopathie et lésions vasculaires), on comprend aisément comment une petite égratignure sur le pied peut provoquer des lésions exagérées, des ulcères hémorragiques qui, à la longue, peuvent induire une gangrène.

Un diabète non contrôlé et dangereusement sous-estimé constitue un risque réel non seulement pour la santé des pieds mais aussi pour la vie même du patient.
Neuropathie et pied diabétique
La neuropathie est extrêmement dangereuse pour les pieds d'un patient diabétique. En présence d'une blessure au pied, le patient - qui ressent moins d'inconfort que l'étendue réelle du dommage ou ne le perçoit pas du tout - continue de mettre du poids sur le pied et de marcher de manière inadéquate : ce comportement aggrave la situation car à partir d'un une petite lésion (comme un cal apparemment inoffensif) crée rapidement une plaie de plus en plus large qui, en dégénérant, forme des ulcères hémorragiques, des infections ou une gangrène.
Un autre élément à ne pas négliger est représenté par déformations du pied, qui peut apparaître avant même l'apparition des symptômes caractéristiques du diabète.Ce trouble est une conséquence de la neuropathie : il y a donc une diminution de la force dans certains groupes de muscles (généralement les antérieurs de la jambe), par conséquent les autres muscles prédominent , provoquant ainsi une rétraction du pied.
Approfondissement
Quels sont les signes avant-coureurs qui peuvent suggérer une mauvaise circulation sanguine chez un diabétique ?
Une suspicion d'approvisionnement en sang pauvre ou pauvre peut survenir lorsque:
- Des épingles et des aiguilles anormales sont ressenties dans les pieds même pendant le repos
- Les crampes dans les jambes surviennent même après une courte marche
- Les petites blessures aux pieds ne peuvent pas guérir facilement
- Les pieds prennent une couleur différente (deviennent plus foncés, rouges, bleus, verts ou noirs)
- Vous avez la sensation d'avoir constamment froid aux pieds
- Des callosités se forment souvent sur la plante du pied ou entre les orteils
D'après ce qui a été dit, il est facile de comprendre comment les pieds et les orteils sont contraints de modifier leur appui au sol ; ainsi les orteils, qui ont tendance à se plier, obligent le pied à supporter des charges de travail anormales et exagérées. La peau fragile du pied, incapable de tolérer les chocs, frottements et traumatismes, se déchire facilement ou est affectée de callosités et d'ampoules qui, si elles ne sont pas traitées à temps, peuvent dégénérer en ulcères.
Pour plus d'informations : Symptômes du pied diabétique
Artériopathie et pied diabétique
Mais pourquoi cela ne se produit-il pas si rapidement dans les pieds d'une personne en bonne santé ?
La dégénérescence rapide en ulcères et infections du pied à partir d'une petite lésion chez un patient diabétique s'explique par une mauvaise circulation dans les membres inférieurs (artériopathie). Les pieds d'un diabétique, ne recevant pas l'apport sanguin nécessaire, luttent pour réparer les dommages que la peau a subis. De plus, la peau du pied diabétique devient fine, fragile et extrêmement délicate (comme la peau d'un enfant), donc plus sujette aux traumatismes et blessures de toutes sortes.
D'autre part, cette dégénérescence rapide des blessures au pied ne se produit pas si souvent chez les sujets sains grâce à la capacité du sang à assurer une circulation sanguine adéquate même au niveau des pieds.
Complications du pied diabétique
Les ulcères du pied sont sans aucun doute la complication la plus fréquente qui survient dans les pieds d'un diabétique. Le danger des ulcères est intimement lié à la mauvaise circulation induite par la maladie artérielle périphérique du diabétique : ne recevant pas la quantité de sang requise, les ulcères peinent à cicatriser.Par conséquent, un mécanisme en cascade se déclenche qui conduit à des hémorragies et/ou des infections. Lorsque l'infection se propage, le patient court le risque de mort des tissus (nécrose des tissus), d'où la gangrène.Dans ce dernier cas, le membre nécessite une intervention médico-chirurgicale immédiate, qui implique l'administration d'antibiotiques pour tuer les bactéries, l'élimination des tissus infectés et, si nécessaire, l'amputation du membre (ou d'une partie de celui-ci) pour éviter les dommages de s'étendant aux quartiers voisins.
Données en main...
D'après les statistiques publiées dans la revue scientifique Le Journal d'Investigation Clinique il est clair que:
- Les ulcères du pied surviennent chez 15 % des diabétiques
- 84 % des amputations des oreillettes inférieures chez les diabétiques sont précisément liées au développement d'ulcères du pied
Le pied diabétique n'est que la partie émergée de l'iceberg, sous lequel il existe une série de problèmes très dangereux qui nécessitent toujours un contrôle et une surveillance médicale.
Autres articles sur "Pied diabétique"
- Pied diabétique : diagnostic, soins et traitement
- Pied diabétique : que faire et ne pas faire