Concepts clés
Là Cellulite infectieuse c'est une « infection bactérienne du tissu conjonctif : c'est une inflammation aiguë et sévère du derme et des couches sous-cutanées.

Les agents responsables les plus impliqués dans la cellulite infectieuse sont les streptocoques et les staphylocoques. Aussi Haemophilus influenzae il peut provoquer des infections similaires, en particulier chez l'enfant. Les patients immunodéprimés sont plus à risque de cellulite infectieuse que les patients sains.
Cellulite infectieuse : symptômes
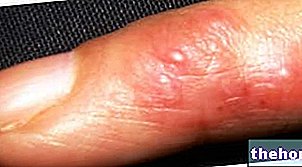
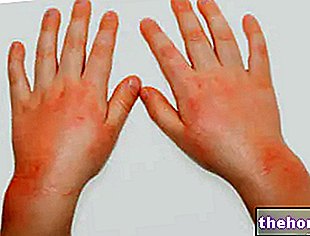
La cellulite infectieuse se manifeste par des rougeurs, une inflammation et des douleurs cutanées au site d'infection. Le patient a souvent de la fièvre. Complications : lymphadénomégalie, lésions papulo-pustuleuses sur la peau, extension de l'infection dans le sang, fasciite nécrosante
Cellulite infectieuse : médicaments
Les antibiotiques sont la thérapie de choix pour le traitement de la cellulite infectieuse.Il est également possible de prendre des analgésiques pour soulager la douleur.
Qu'est-ce que la cellulite infectieuse ?
Cellulite infectieuse : définition
La cellulite infectieuse est un "infection bactérienne assez commun et dangereux de la tissu conjonctif, caractérisée par une inflammation sévère de la peau et des couches sous-cutanées.
A ne pas confondre avec la cellulite cosmétique, la cellulite infectieuse est déclenchée par une insulte bactérienne: au site d'infection, la peau apparaît rouge, enflammée, chaude et douce au toucher.La cellulite infectieuse a tendance à se propager rapidement, infectant également le autres sites anatomiques: lorsqu'elle n'est pas traitée, "l'infection peut mettre la vie du patient en danger. D'après cela, il est compréhensible que la cellulite bactérienne constitue un"urgence médicale à tous égards.
Malgré le danger de la maladie, le traitement est assez simple : une antibiothérapie spécifique élimine l'agent causal, favorisant la guérison complète du patient.
En raison des multiples affinités, la cellulite infectieuse est souvent confondue avec « l'érysipèle : une infection bactérienne aiguë de la peau impliquant le derme, des couches plus superficielles de l'hypoderme et des vaisseaux lymphatiques (elle est donc plus superficielle que la cellulite infectieuse). Cependant, de nombreux patients sont hospitalisés. atteints de cellulite infectieuse sont touchés aussi de l'érysipèle.
Causes et facteurs de risque
Cellulite infectieuse : quelles en sont les causes ?
La cellulite infectieuse est l'expression d'une agression bactérienne : les agents pathogènes pénètrent dans la peau par des micro-lésions ou des plaies étendues.
Les bactéries les plus impliquées dans la cellulite bactérienne sont :
- Streptocoques (Streptocoque pyogène bêta hémolytique du groupe A);
- Staphylocoques (Staphylococcus aureus) : ces dernières années, des cas de cellulite bactérienne médiée par la bactérie MRSA (acronyme de Methicilline-résistant Staphylococcus aureus). C'est un staphylocoque résistant aux antibiotiques bêta-lactamines, dont les pénicillines et les céphalosporines.
Les Streptocoques et Staphylocoques sont les agents infectieux les plus impliqués dans la cellulite bactérienne ; cependant, d'autres bactéries aérobies et anaérobies peuvent également déclencher une infection.
Chez le bébé, la cellulite infectieuse peut aussi être causée par la bactérie Haemophilus influenzae.
Cellulite infectieuse : facteurs de risque

La cellulite bactérienne peut affecter n'importe qui ; cependant, les patients immunodéprimé représentent la catégorie la plus à risque.
L'affaiblissement du système immunitaire peut être favorisé par les leucémies, les infections à VIH, les maladies rénales chroniques, les maladies du foie, les troubles de la circulation sanguine et le diabète.L'abus de certains médicaments (corticoïdes) affaiblit également le système immunitaire.
Certains ont également été identifiés maladies prédisposantes cellulite infectieuse; parmi ceux-ci on se souvient :
- Feu de S. Antonio;
- Varicelle;
- Eczéma;
- Pied d'athlète;
- Lymphœdème : le gonflement des articulations rend la peau plus sensible aux infections ;
- Obésité : le risque à la fois de la cellulite infectieuse et de ses formes récidivantes augmente.
Symptômes et complications
Pour en savoir plus : Symptômes Cellulite infectieuse
Cellulite infectieuse : comment se manifeste-t-elle ?
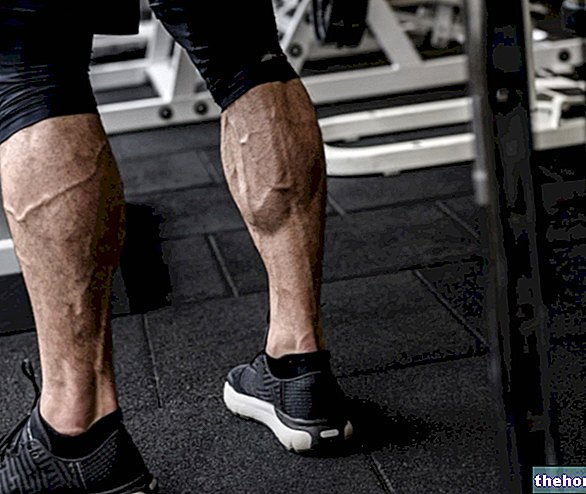
La cellulite infectieuse peut toucher n'importe quelle partie du corps ; néanmoins, le jambes inférieures constitue la cible la plus courante de l'infection.
Au site d'infection, la peau est chaude et douce au toucher, douloureuse, enflée et rouge.
La formation de stries rougeâtres particulières sur la peau est une indication de la propagation bactérienne dans les vaisseaux lymphatiques : dans des circonstances similaires, la cellulite bactérienne favorise la formation de lymphadénomégalie.
Il n'est pas rare qu'un patient atteint de cellulite bactérienne subisse un changement soudain de la température basale (fièvre).
Le tableau clinique du patient atteint de cellulite infectieuse peut se compliquer au point de former des lésions papulo-pustuleuses sur la peau. Dans les cas graves, les bactéries peuvent infecter le sang (bactériémie).
Là fasciite nécrosante c'est une complication possible de la cellulite bactérienne : c'est une inflammation rare d'étiologie infectieuse, impliquant les couches profondes de la peau et des tissus sous-cutanés. La fasciite nécrosante, s'étendant rapidement à travers le tissu conjonctif, constitue une « urgence médicale ».
Diagnostic et traitement
Quels tests permettent de diagnostiquer la cellulite infectieuse ?
L"anamnèse et le "examen physique ils sont indispensables pour un premier diagnostic approximatif. La suspicion de cellulite infectieuse peut être confirmée par analyse de sang.
Là diagnostic différentiel il est important de distinguer la cellulite infectieuse des autres affections similaires :
- Une « échographie des veines des membres inférieurs détecte la présence éventuelle d'un caillot sanguin → diagnostic différentiel avec thrombose veineuse profonde ;
- Une radiographie aux rayons X constate ou nie la propagation de la cellulite infectieuse aux os;
- Le diagnostic différentiel doit également être fait avec la maladie de Lyme.Le test sanguin peut ou non confirmer cette anthropozoonose. Normalement, le test ci-dessus est recommandé dans les pays où la maladie est endémique, en particulier pendant les mois d'été.
Là biopsie cutanée ou je "examen culturel (hémoculture) ne sont généralement pas nécessaires : en effet, il n'est pas si immédiat d'isoler le pathogène impliqué dans la cellulite infectieuse.
Cellulite infectieuse : quelle est la thérapie attendue ?
Les traitement antibiotique de la cellulite bactérienne devrait commencer dans les plus brefs délais à partir de la manifestation des tout premiers symptômes. Pour les formes bénignes, l'administration orale ou intraveineuse de médicaments tels que la flucloxacilline ou la dicloxacilline est suffisante. Les variantes modérées et sévères sont traitées avec de la phénoxyméthylpénicilline par voie orale (un médicament également indiqué pour le traitement de l'érysipèle); en alternative, administrer de la benzylpénicilline par voie intraveineuse ou de l'ampicilline/amoxicilline.
La cellulite infectieuse s'accompagne souvent de douleur et irritation locales: pour faire face à la perception douloureuse constante, l'administration d'une thérapie de soutien (ex. AINS) est recommandée.
Dans la plupart des cas, les symptômes de la cellulite infectieuse disparaissent 24 à 48 heures après l'administration d'antibiotiques. Cependant, il est recommandé de conclure le cycle thérapeutique, même en cas de rémission complète des symptômes, quelques jours après le début du traitement : en complétant l'antibiothérapie, le risque de récidive de cellulite infectieuse est minimisé.
Voir aussi : Médicaments pour le traitement de la cellulite infectieuse »

-cause-sintomi-e-cura.jpg)