La fréquence cardiaque est l'un des paramètres corporels les plus importants, car elle est directement liée à la fonction vitale du cœur. Elle peut augmenter ou diminuer pour réguler la circulation sanguine, en réponse à divers types de stimuli ou pour effectuer des « compensations » physiologiques ; certaines modifications importantes sont plutôt interprétées comme des symptômes pathologiques.
Des exemples typiques de variation "normale" de la fréquence cardiaque sont liés à : l'activité physique, la pression artérielle, la fréquence respiratoire ou la libération d'hormones-neurotransmetteurs tels que les catécholamines. L'augmentation physiologique de la fréquence cardiaque est un moyen d'apporter plus de sang, donc plus d'oxygène, aux tissus.
, même si cela ne nécessite pas de soins médicaux particuliers ; en outre, cela pourrait être un problème, même s'il y a de nombreux athlètes avec moins de 50 bpm sans aucun symptôme ou conditions inconfortables. Entre 90 et 100, la valeur est toujours considérée comme normale, mais des taux persistants entre 80 et 100 bpm, en particulier pendant le sommeil, peuvent être des signes d'hyperthyroïdie ou d'anémie. En plus de 100 bpm on parle de tachycardie.
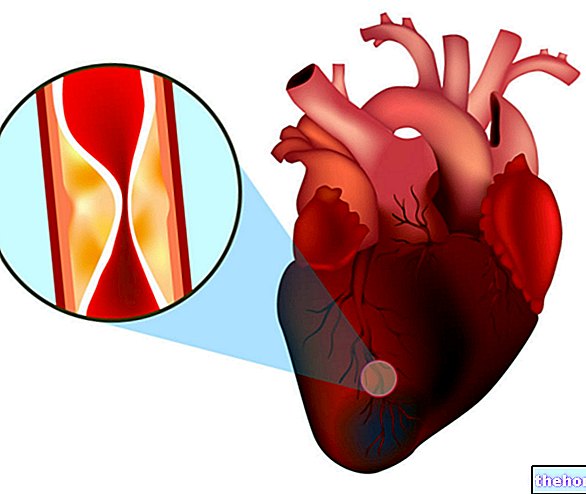
Une « fréquence cardiaque au repos élevée est associée à une augmentation de la mortalité cardiovasculaire et toutes causes confondues dans la population générale et chez les patients atteints de maladies chroniques. Une fréquence cardiaque au repos plus rapide est donc associée à une espérance de vie plus courte et est considérée comme un facteur de risque important de les maladies cardiaques et l'insuffisance cardiaque, quel que soit le niveau de forme physique. Il a été démontré qu'une fréquence cardiaque au repos supérieure à 65 bpm a un effet important, bien qu'indépendant, sur la mortalité prématurée ; il a été démontré qu'une augmentation de 10 battements par minute de la FC au repos est associée à un risque accru de décès de 10 à 20 %. Les hommes sans signes de maladie cardiaque et dont la fréquence cardiaque au repos est supérieure à 90 bpm ont un risque cinq fois plus élevé de mort subite d'origine cardiaque. Les hommes dont la fréquence cardiaque au repos est supérieure à 90 bpm ont un risque presque double de mortalité par maladie cardiovasculaire ; chez les femmes, l'augmentation est même triple.
Les changements de mode de vie et les thérapies médicamenteuses peuvent être utiles pour réduire les fréquences cardiaques au repos élevées. L'exercice est une mesure potentiellement utile et à considérer lorsque la fréquence cardiaque au repos d'un individu est supérieure à 80 bpm. L'alimentation s'est également avérée bénéfique pour réduire la fréquence cardiaque au repos : dans les études de FC au repos et le risque de décès et de complications cardiaques chez les patients avec le diabète de type 2, il a été démontré que la consommation de légumineuses réduisait la fréquence cardiaque au repos. On pense que cela se produit car, en plus d'avoir des effets bénéfiques directs, ces aliments affectent la réduction des graisses saturées et du cholestérol.
Quelle que soit la prédisposition individuelle, le sport aérobie pratiqué depuis de nombreuses années et avec des charges de travail importantes a tendance à réduire la FC, aussi bien au repos qu'à l'activité.Au contraire, les disciplines de haute intensité (HIT) permettent de maintenir la capacité d'atteindre des battements par minute très élevés en efforts maximaux et sous-maximaux.
La fréquence cardiaque au repos peut également être affectée par certains médicaments ; par exemple, les stimulants tels que les amphétamines ont tendance à l'augmenter, tandis que les sédatifs et les antidépresseurs aident à la réduire.
La fréquence cardiaque est mesurée aussi bien au repos qu'à l'effort, en fonction de l'investigation à réaliser ; si la première fait partie intégrante de tout examen médical de base, ce dernier cas est particulièrement référé au contrôle de la condition physique sportive de compétition.
accélérateurs cardio
Facteurs qui réduisent la fréquence cardiaque et la force de contraction
La méthode la plus simple est la méthode instrumentale, car elle minimise l'erreur liée à l'opérateur.
Les appareils qui permettent de mesurer la fréquence cardiaque au repos sont : le cardiofréquencemètre (poitrine ou poignet), l'oxymètre de pouls, le sphygmomanomètre électronique (non manuel, qui nécessite plutôt des compétences d'utilisation spécifiques) et le stéthoscope.
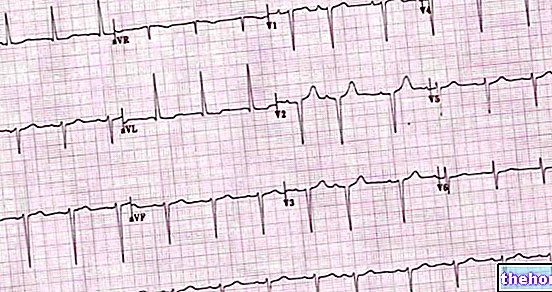
L'électrocardiogramme remplit également cette fonction, cependant dédiée à des investigations diagnostiques plus complexes, généralement réalisées dans le secteur de la santé et par du personnel compétent.
Comment mesurer la fréquence cardiaque au repos sans cardiofréquencemètre ?
La mesure de la fréquence cardiaque au repos s'effectue en palpant l'artère radiale (au poignet) ou l'artère carotide (au cou), en sentant le changement de pression sur le bout des doigts. Le laps de temps idéal est d'une minute entière, pendant laquelle il faut compter les battements avec précision.Il est bon de rappeler que la force appliquée doit être légère, surtout en correspondance avec l'artère carotide.
Alternativement, il est possible de détecter les pulsations de manière segmentée, par exemple toutes les 10, 15 ou 20 secondes, en les notant dans un tableau et en extrapolant la valeur finale à la fin (en multipliant x 6 dans le premier cas, x 4 dans le deuxième et x 3 dans le troisième).